US Pharm. 2019;44(4):31-34.
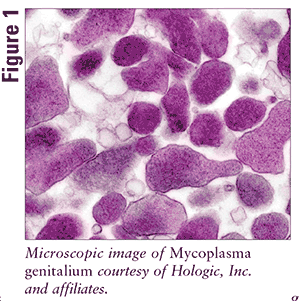
Mycoplasma genitalium (FIGURE 1) was discovered in 1981 and identified as the smallest (0.1-0.5 micrometer) organism of record. It is a one-cell, viable form of the Mycoplasma species, devoid of a peptidoglycan cell wall, and the 12th Mycoplasma species. Research shows that M genitalium, though structurally and antigenically related to Mycoplasma pneumoniae, has different genomic characteristics when compared with M pneumoniae. Other characteristics of M genitalium include the organism’s ability to adhere to glass, plastic surfaces, and particularly to epithelial cells; its gliding motility and slow growth; and its bottle- or pear-shaped structure with a rod-like head.1-3
This organism was initially identified from studying nongonococcal urethritis in men, and it was subsequently isolated from the urogenital tract of heterosexual men and women and in perianal areas of men who have sex with other men (MSM).1,4-13 The organism has been reported to be more common in men with urethritis and MSM.6,7,12,13 M genitalium has been reported to cause balanosposthitis in men, and urethritis, cervicitis, pelvic inflammatory disease (PID), and infertility in women.9,14,15 It has also been isolated from the sperm of men with urethritis, but it is not known if it causes infertility in men.16 Additionally, there are at least two reported cases in which the organism was isolated from the synovial fluid of patients with arthritis.17
Epidemiology
The CDC reports that 15% to 30% of urethritis in men and 10% to 30% of cervicitis cases are caused by M genitalium. The organism is now reported to be more prevalent than Neisseria gonorrheae and second only behind Chlamydia trachomatis in causing the most sexually transmitted infections (STIs) in the United States.18 Fifty percent of M genitalium–related cases in women may be resistant to macrolide antibiotics, while 42% of cases involving the organism in men are reported to be macrolide-resistant.19
Clinical Signs, Symptoms, and Complications
Although M genitalium infections can be asymptomatic, patients may present with symptoms traditionally associated with other bacterial urinary tract infections (UTIs) and STIs. Symptoms include, but are not limited to, burning, stinging and pain on urination, watery discharge in men and women, painful sex, bleeding after sex, and pelvic pain.10
The most common complications reported are urethritis, cervicitis, PID, and infertility.1,11,14,20 In fact, M genitalium is responsible for 2% to 22% of PID, which may affect fertility in women, and is present in 10% to 30% of women diagnosed with cervicitis.21-24 Though inflammation can cause difficulty for women of child-bearing age to become pregnant, it is not known if men may become infertile as a result of infection.16,25 Additionally, it has been postulated that M genitalium may be associated with an increased risk of human immunodeficiency viral infections.26,27
Diagnosing Mycoplasma genitalia With the Aptima Assay
The detection of Mycoplasma species using traditional microbiological tests has been difficult, and it can take as long as 6 months to culture the organism.18 Adhesion patterns and the slow-growing nature of this organism make it difficult to identify quickly and perform antimicrobial-susceptibility testing. This behavior makes treatment more difficult and, in certain cases, can lead to antimicrobial resistance and treatment failure. Since the 1980s, the test used to diagnose mycoplasma genitalia (MG) was the nucleic acid amplification test (NAAT), which was made easier by the use of polymerase chain reaction (PCR) in the 1990s.28 NAAT PCR is currently available only in reference laboratories and is not readily available to small hospitals and clinics.
Diagnosis has become less cumbersome due to the advent of the Aptima Mycoplasma genitalium Assay (FIGURE 2). On January 23, 2019, the FDA announced that it permitted marketing for the first-ever MG-specific test to assist in the diagnosis of this increasingly burdensome infection.29 Prior to granting approval, the FDA reviewed clinical studies involving 11,774 samples containing the organism. The ribosomal, RNA-based assay showed greater sensitivity than the previous tests and identified the organism in 90% of samples. Approximately 78% of samples from female urine were identified with 99% specificity and 90.9% from male urine with a specificity of 99.4%. Percent specificity of vaginal, endocervical, and meatal swabs was 98%, 98.4%, 97.8%, respectively. Cross-reactivity was studied to determine if other organisms could affect the result of the test, and it was shown that there was no cross-reactivity and/or significant interactions with other organisms.30,31
The availability of this test will confirm 90% of urine and swab samples from regions affected, such as the cervix, urethra, and vagina. Once detected, physicians will be able to target the organism for more specific treatment and may ultimately achieve better outcomes. The special control established by the FDA ensures the safety and effectiveness of the test.
Disease-Detection Specificity
The Aptima Mycoplasma genitalium Assay is a revolutionary assay specifically intended to detect M genitalium.31 Though this test also involves the NAAT principles, it also has target capture, transcription-mediated amplification, and hybridization protection assay technologies that recognize the M genitalium cRNA. Results are automatically interpreted as valid by the Panther system Aptima Mycoplasma genitalium Assay software. They are subsequently recorded as negative, positive, or invalid, if an error occurs. Invalid results require retesting of the specimens. Specimens can be kept under recommended conditions for up to 90 days.
According to the CDC, greater than 15% of male and female patients with nongonococcal STIs are at risk of acquiring MG, and its incidence is increasing.18,19 Undiagnosed and misdiagnosed cases of M genitalium infections may be one of the primary factors leading to untreated cases, suboptimal therapy, severe complications such as infertility, and the development of resistance to currently available antibiotics. The assay will curtail misdiagnoses and will assist with more rapid detection of the bacteria. As a result, more timely, accurate, and cost-effective therapy can be initiated.
Healthcare Personnel Training
Personnel must be trained in the use and handling of the test and all its components, including specified disposable laboratory personnel–protective equipment.31 Specimens must be handled with care as they may be infectious. Proper collection, handling, and storage at specified temperature using universal precautions are recommended with instructions provided in the test kit package insert. Personnel involved are warned that the content of the test kit can be corrosive to skin, eyes, and other mucous membranes. All areas exposed to the irritant must be washed with water thoroughly before drying the area. The Panther System Operator’s Manual should be reviewed for all additional warnings and precautions associated with this test. A Safety Data Sheet Library, which provides additional information on hazard and precautionary statements, is also available at www.hologicsds.com.
Limitations of the Assay
The possibility of infection may still exist, even in the absence of positive results. The manufacturer recommends that test results be used in conjunction with clinical and other laboratory data. The manufacturer also recommends that vaginal swabs be used in all females suspected of MG, as urine samples and endocervical swabs may not always capture the presence of the organism. When vaginal swab samples are not available, urine samples and cervical swabs can be used as alternatives.31
Treatment
The bacterium lacks a cell wall and does not respond to penicillins and cephalosporins. Therefore, drugs such as macrolides, quinolones, and other agents that inhibit protein synthesis are currently used as treatment options.
Empiric treatment must be started immediately until identification is made. Empiric therapy recommended for MG includes azithromycin 1 gram or 1.5 gram × 1 dose or a 500-mg initial dose followed by 250 mg daily for 4 days. The single dose of azithromycin is more likely to lead to treatment failure than the extended 5-day therapy.32,33 For patients who do not respond to azithromycin, moxifloxacin 400 mg by mouth daily for 7, 10, or 14 days is recommended.18
Development of resistance to these antibiotics has made treatment very difficult. Agents that have shown positive outcomes in patients who are resistant to both azithromycin and moxifloxacin are pristinamycin, solithromycin, and spectinomycin.34-38 Pristinamycin is a combination agent containing pristinamycin IA, a macrolide-like streptogramin B, and pristinamycin IIA, which is a macrolide. Both agents inhibit protein synthesis by binding to the 50S ribosomal subunits and are bacteriostatic. However, when combined, they provide synergistic, bactericidal activity against M genitalium.35,36 Solithromycin, a fluoroketolide antibiotic, and spectinomycin, an aminoglycoside, have also been found to be effective in treatment-resistant organisms.37,38 Several other agents are currently being investigated for treatment, including omadacycline, linezolid, and sitafloxacin.39
Management of Sex Partners and Prevention
It is important for all sexual partners—men and women, heterosexuals, and MSM—to be tested and treated appropriately. Treatment of sex partners reduces the rate of reinfection and the development of resistance to current therapy.
In addition to the treatment of sexual partners, some patients are advised to be retested after completion of therapy to ensure eradication of the organism. Methods of prevention include the use of condoms, abstinence during active infection, and routine sexual checkups to limit the complications of the infection and the probability of contracting other STIs.18
Conclusion
Though prior diagnosis options have been challenging, the advent of the Aptima Mycoplasma genitalium Assay made the road to optimal therapy easier by increasing the likelihood of early diagnosis and the subsequent institution of effective treatment modalities. More studies are warranted to further investigate the incidence of M genitalium–positive infections, and newer antibiotics specific to the treatment of MG need to be developed.
More information about the Aptima Mycoplasma genitalium Assay can be found at https://healthdxs.com/en. Hologic, Inc. is a medical technology company that specializes in the detection of diseases and treatment of women and the optimization of women’s health. More information about this company and its technology commitment can be found at www.hologic.com.
REFERENCES
1. Tully JG, Taylor-Robinson D, Cole RM, et al. A newly discovered mycoplasma in the human urogenital tract. Lancet. 1981;1:1288-1291.
2. Colman SD, Hu P-C, Litaker W, et al. A physical map of the Mycoplasma genitalium genome. Mol Microbiol. 1990;4:683-687.
3. Taylor-Robinson D, Bredt W. Motility of mycoplasma strain G37. Yale J Biol Med. 1983;56:910.
4. Jensen JS, Hansen HT, Lind K. Isolation of Mycoplasma genitalium: an emerging cause of sexually transmitted strains in the male urethra. J Clin Microbiol. 1996;34(2):286-291.
5. Horner P, Martin D. Mycoplasma genitalium infection in men. J Infect Dis. 2017;216(suppl 2):S396.
6. Hooton TM, Roberts MC, Roberts PL, et al. Prevalence of Mycoplasma genitalia determined by DNA probe in men with urethritis. Lancet. 1988;1:266-268.
7. Jensen JS, Orsum R, Dohn B, et al. Mycoplasma genitalium: a cause of male urethritis? Genitourin Med. 1993;69:265-269.
8. McGowin CL, Anderson-Smits C. Mycoplasma genitalium: an emerging cause of sexually transmitted disease in women. PloS Pathog. 2011;7(5):e1001324.
9. Lis R, Rowhani-Rahbar A, Manhart LE. Mycoplasma genitalium infection and female reproductive tract disease: a meta-analysis. Clin Infect Dis. 2015;61(3):418-426.
10. Falk L, Fredlund H, Jensen JS. Signs and symptoms of urethritis and cervicitis among women with or without Mycoplasma genitalium or Chlamydiae trachomatis infection. Sex Transm Infect. 2005;81(1):73-78.
11. Manhart LE, Critchlow CW, Holmes KK, et al. Mucopurulent cervicitis and Mycoplasma genitalium. J Infect Dis. 2003;187(4):650-657.
12. Soni S, Alexander S, Verlander N, et al. The prevalence of urethral and rectal Mycoplasma genitalium and its associations in men who have sex with men attending a genitourinary medicine clinic. Sex Transmit Infect. 2010;86:21-24.
13. Taylor-Robinson D, Gilroy CB, Keane FE. Detection of several Mycoplasma species at various anatomical sites of homosexual men. Eur J Clin Microbiol Infect Dis. 2003;22(5):291-293.
14. Horner PJ, Taylor-Robinson D. Association of Mycoplasma genitalium with balanosposthitis in men with non-gonococcal urethritis. Sex Transm Infect. 2011;87(1):38-40.
15. Moller BR, Taylor-Robinson D, Furr PM. Serologic evidence implicating Mycoplasma genitalia in pelvic inflammatory disease. Lancet. 1984;1:1102-1103.
16. Svenstrup HF, Fedder J, Abraham-Peskir, et al. Mycoplasma genitalium attaches to human spermatozoa. Hum Reproduct. 2003;18(10):2103-2109.
17. Taylor Robinson D, Gilroy CB, Horowitz S, Horowitz J. Mycoplasma genitalium in the joints of two patients with arthritis. Eur J Clin Microbiol Infect Dis. 1994;13(12):1066-1069.
18. CDC. 2015 Sexually Transmitted Diseases Treatment Guidelines. Emerging Issues. www.cdc.gov/std/tg2015/emerging.htm. Updated June 4, 2015. Accessed January 23, 2019.
19. Getman D, Jiang A, O’Donnell M, et al. Mycoplasma genitalium prevalence, coinfection, and macrolide antibiotic resistance frequency in a multicenter clinical study cohort in the United States. J Clin Microbiol. 2016;54(9):2278-2283.
20. Manhart LE, Holmes KK, Hughes JP, et al. Mycoplasma genitalium among young adults in the United States: an emerging sexually transmitted infection. Am J Public Health. 2007;97(6):1118-1125.
21. Lu GC, Schwebke JR, Duffy LB, et al. Midtrimester vaginal Mycoplasma genitalium in women with subsequent spontaneous preterm birth. Am J Obstet Gynecol. 2001;185(1):163-165.
22. Cohen CR, Manhart LE, Bukusi EA, et al. Association between Mycoplasma genitalium and acute endometritis. Lancet. 2002;359(9308):765-766.
23. Oakeshott P, Hay P, Taylor-Robinson D, et al. Prevalence of Mycoplasma genitalium in early pregnancy and relationship between its presence and pregnancy outcome. BJOG. 2004;111(12):1464-1467.
24. Rajkumari N, Kaur H, Roy A, et al. Association of Mycoplasma genitalium with infertility in North Indian women. Indian J Sex Transm Dis. 2015;36(2):144-148.
25. Huang C, Zhu HL, Xu KR, et al. Mycoplasma and ureaplasma infection and male infertility: a systematic review and meta-analysis. Andrology. 2015;3(5):809-816.
26. Vandepitte J, Weiss HA, Bukenya J, et al. Association between Mycoplasma genitalium infection and HIV acquisition among female sex workers in Uganda: evidence from a nested case-control study. Sex Transm Infect. 2014;90(7):545-549.
27. Manhas A, Sethi S, Sharma M, et al. Association of genital mycoplasmas including Mycoplasma genitalium in HIV infected men with nongonococcal urethritis attending STD & HIV clinics. Indian J Med Res. 2009;129(3):305-310.
28. Jensen JS, Uldum SA, Sondergard-Andersen J, et al. Polymerase chain reaction for detection of Mycoplasma genitalium in clinical samples. J Clin Microbiol. 1991;29(1):46-50.
29. FDA news release. FDA permits marketing of first test to aid in the diagnosis of a sexually-transmitted infection known as Mycoplasma genitalium. January 23, 2019. www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm629746.htm. Accessed March 26, 2019.
30. Unemo M, Salado-Rasmussen K, Hansen M, et al. Clinical and analytical evaluation of the new Aptima Mycoplasma genitalium Assay, with data on M. genitalium prevalence and antimicrobial resistance in M. genitalium in Denmark, Norway and Sweden in 2016. Clin Microbiol Inf. 2018;24:533-539.
31. Hologic documents. www.hologicsds.com. Accessed January 23, 2019.
32. Horner P, Blee K, Adams E. Time to manage Mycoplasma genitalium as an STI: but not with azithromycin 1 g!. Curr Opin Infect Dis. 2014;27(1):68-74.
33. Read TR, Fairley CK, Tabrizi SN, et al. Azithromycin 1.5g over five days compared to 1g single dose in urethral Mycoplasma genitalium: impact on treatment outcome and resistance. Clin Infect Dis. 2017;64:250-256.
34. Hamasuna R, Le PT, Kutsuna S, et al. Mutations in ParC and GyrA of moxifloxacin-resistant and susceptible Mycoplasma genitalium strains. PLoS One. 2018;13:e0198355.
35. Mast Y, Wohlleben W. Streptogramins—two are better than one! Int J Med Microbiol. 2014;304:44-50.
36. Read T, Jensen JS, Fairley CK, et al. Use of pristinamycin for macrolide-resistant Mycoplasma genitalium infection. Emerg Infect Dis. 2018;24(2):328-335.
37. Jensen JS, Fernandes P, Unemo M. In vitro activity of the new fluoroketolide solithromycin (CEM-101) against macrolide-resistant and -susceptible Mycoplasma genitalium strains. Antimicrob Agents Chemother. 2014;58:3151-3156.
38. Falk L, Jensen JS. Successful outcome of macrolide-resistant Mycoplasma genitalium urethritis after spectinomycin treatment: a case report. J Antimicrob Chemother. 2017;72(2):624-625.
39. Bradshaw C, Jensen JS, Waites KB. New horizons in Mycoplasma genitalium treatment. J Infect Dis. 2017;216(suppl 2):S412-S419.





