US Pharm. 2019;44(10)4-8.
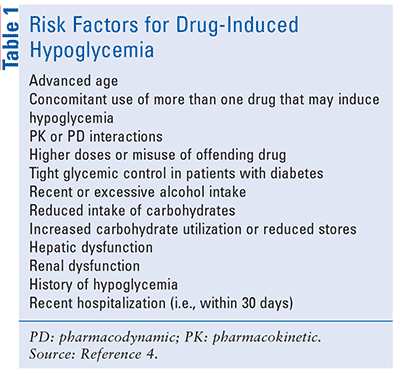
There is much to be learned from those who have examined the unintended effects of medication therapy. As this knowledge base increases, it is important to seek systematic reviews and meta-analyses of these effects and to rely on the evidence these studies provide in order to better serve patients through appropriate medication monitoring and other medication-therapy management (MTM) services. In light of the fact that advancing age is a risk factor for drug-induced (DI) hypoglycemia (TABLE 1), this brief discussion will provide nuanced guidance and additional resources to help pharmacists better individualize pharmaceutical care to this vulnerable patient population.
A DI disease is the unintended effect of a drug that results in mortality or morbidity with symptoms sufficient to prompt a patient to seek medical attention and/or potentially require hospitalization. Hypoglycemia, or low blood sugar, can be defined by the glucose-alert value of less than or equal to 70 mg/dL (3.9 mmol/L).1,2 Varying blood-glucose levels can cause typical symptoms of hypoglycemia (e.g., shakiness, sweating, fatigue, hunger, headaches, and confusion) in individuals with diabetes mellitus.3 While DI hypoglycemia typically causes mild-to-moderate transient symptoms (TABLE 2), a level of discomfort and reduction in quality of life may reach a point that causes a patient to become nonadherent with a medication or regimen in an attempt to avoid repeated episodes.4 Furthermore, there is a significant economic burden associated with DI glucose and insulin dysregulation, owing to the expense of urgent-care visits and hospitalizations related to treatment of hypoglycemia and hypeglycemia.
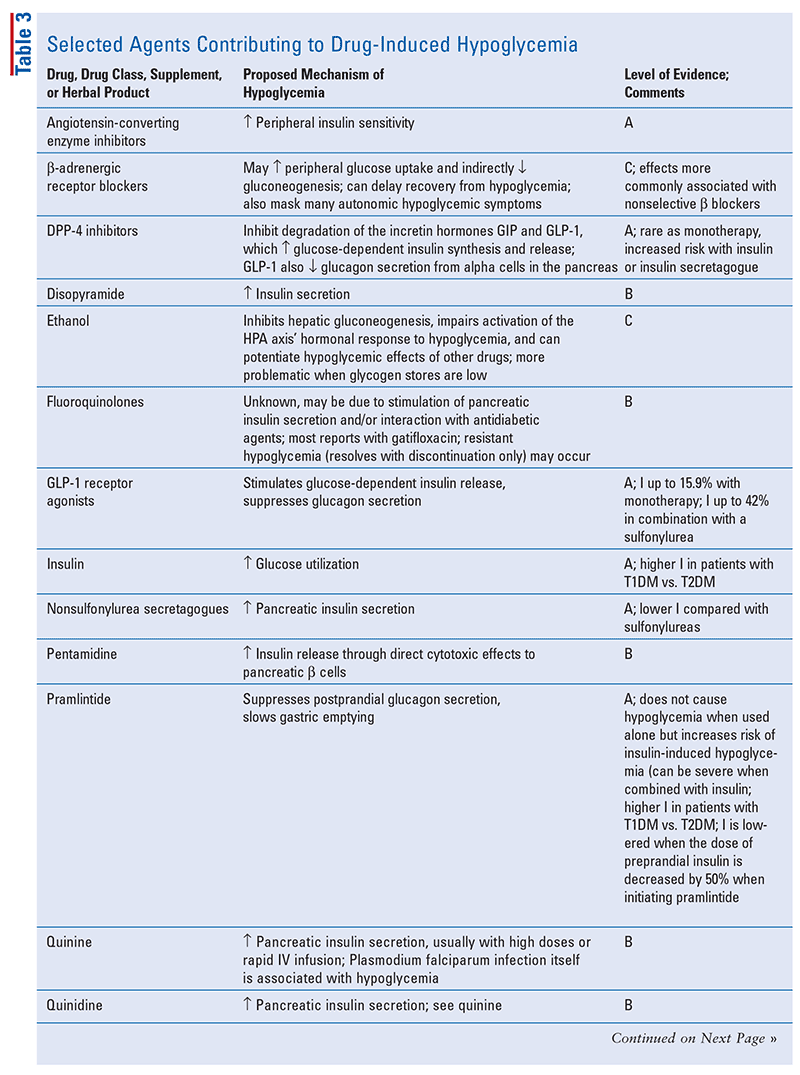
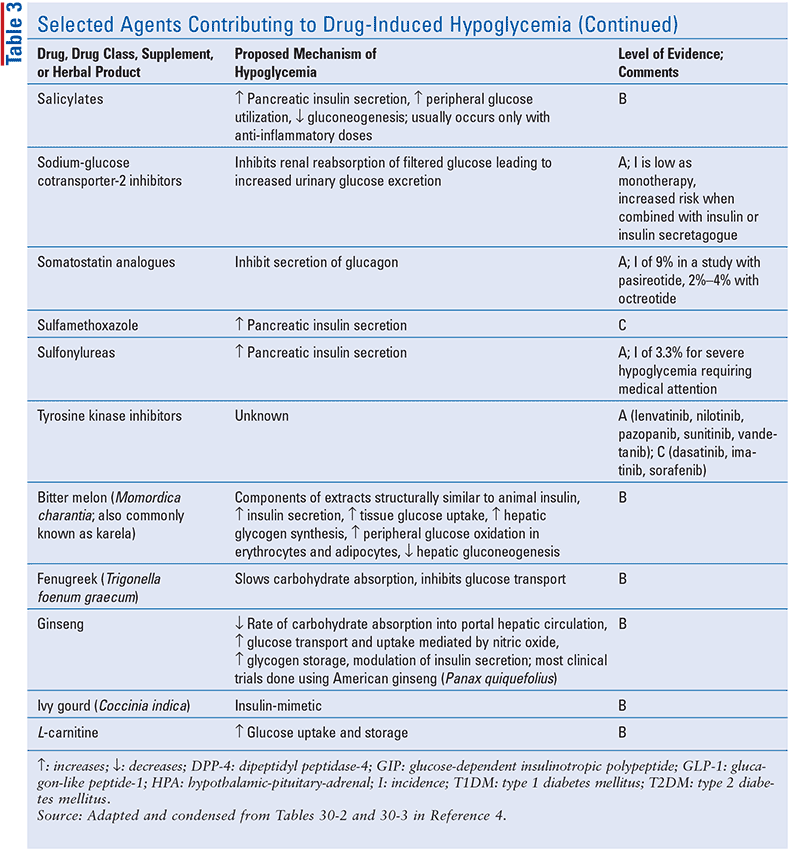
Before implicating a drug as the cause of DI hypoglycemia (TABLE 3), other possible etiologies (e.g., alcohol-use disorder, sepsis, hepatic failure, large non–beta-cell tumor) must be ruled out; for the differential diagnoses for DI hypoglycemia, see RESOURCES.
Effectively Communicating Signs and Symptoms
For those patients receiving medications known to cause hypoglycemia, providing education regarding the associated signs and symptoms, the importance of follow-up testing, and the need for careful management and close medical supervision is imperative. In doing so, it is important to consider the health literacy of each patient so that good communication, which is necessary for patient-centered care, adequately addresses the patients’ needs and wants.5 Terminology regarding the signs and symptoms of DI hypoglycemia must be commensurate with the patient’s health-literacy level. For example, the symptom of anxiety may in some cases be better communicated as “feeling nervous” and the symptom of irritability may be described as “moodiness,” if appropriate (see RESOURCES). The importance of this nuanced approach to communication—particularly for older adults, in conjunction with education and appropriate prescribing—is underscored by reports that adverse drug events account for 30% of hospital admissions for persons aged 65 years and older, and between 15% and 65% of these events are preventable by avoiding potentially inappropriate medications, communicating effectively, and educating patients.6,7
Mechanisms of Drug-Induced Glucose and Insulin Imbalance
While an organic imbalance between plasma glucose and insulin concentration can result in hyperglycemia or hypoglycemia, drugs may also induce hyperglycemia or hypoglycemia via mechanisms as varied as4:
• Alterations of insulin secretion and sensitivity
• Changes in gluconeogenesis, and
• Direct cytotoxic effects on pancreatic beta cells
When the etiology of hyperglycemia or hypoglycemia is DI, the condition can progress to consequential manifestations, including diabetes mellitus, severe hypoglycemia, coma, and death. When healthcare practitioners are aware of this potential medication-related problem and provide close monitoring and judicious use of the suspected drugs, adverse events such as these can be prevented and/or minimized.4
Advancing Age: Polypharmacy,
Nonadherence, Unintended Weight Loss
Older adult patients often have multiple medications, multiple comorbidities, and multiple prescribers.8 Polypharmacy associated with clinical practice guidelines for older adults, an individual patient’s self-management through the use of OTC medications, herbal products, and supplements can complicate the regimen of an older adult and need to be thoroughly considered, evaluated, and modified as appropriate.7
There should be special geriatric consideration regarding a decision to initiate certain drugs (i.e., particularly those agents in which coadministration with insulin may induce severe hypoglycemia [e.g., pramlintide]) in the older-adult population; such a decision should be carefully based on several factors, including the patient’s functional status and how well the patient recognizes hypoglycemic and hyperglycemic symptoms and how to respond to them.9
Additionally, as mentioned above, symptom manifestation and a subjective reduction in quality of life that a patient attributes to medication therapy (e.g., adverse drug effects, troublesome administration, tedious and uncomfortable monitoring) can also contribute to medication nonadherence. In an older adult, addressing deficits in vision and hearing, swallowing and motor impairment, cognition, and health literacy can lead to enhanced medication adherence.8 It should also not be overlooked in the elderly that unintended weight loss (e.g., secondary to malignancy) may be an insidious precipitator of hypoglycemia.
Hypoglycemia Following Gastric-Bypass Surgery
Patients who have undergone gastric bypass surgery commonly experience nonspecific postprandial symptoms attributable to hypoglycemia.10 There is a more severe postprandial hypoglycemia—hyperinsulinemic hypoglycemia; however, that may present several months to years (usually more than 1 year) after gastric bypass surgery; while rare, the hallmark is severe postprandial neuroglycopenia (in contrast to dumping syndrome, which is noted soon after the surgery and improves with time).10
Management
Strategies for managing DI glucose and insulin dysregulation are presented in Reference 4; those strategies specific to the management of DI hypoglycemia include:
• Administer treatment to reverse hypoglycemia as appropriate (e.g., glucose, dextrose, glucagon, diazoxide)
• Assess glycemic control (e.g., fasting plasma glucose concentration) as appropriate
• Discontinue or reduce dose of offending drug if possible
• Modify diet as appropriate (e.g., frequent, small meals)
• Use offending drug at the lowest effective dose for shortest duration possible
Patient education, including MTM interactions, should include comprehensive teaching of appropriate management strategies involving patients and their families and caregivers.
Prevention of Drug-Induced Glucose and Insulin Imbalance
A risk-benefit evaluation should be considered for each individual patient, bearing in mind that in a high-risk patient, avoidance of potentially causative drugs may be the best preventive strategy, although not always possible. The following general preventive strategies have been recommended4:
Avoid Concomitant Use of: more than one drug that can cause glucose and/or insulin dysregulation; drugs that could cause pharmacokinetic or pharmacodynamic drug interactions with a potentially causative drug.
At Each Visit: Inquire about any symptoms of hypoglycemia or hyperglycemia; monitor weight.
Monitor Fasting Plasma-Glucose Concentration: within the first few weeks following the initiation of high-risk drugs, and regularly thereafter, particularly in the presence of weight changes or preexisting disorders of glucose metabolism; in addition to postprandial plasma-glucose concentration monitoring, for patients taking glucocorticoids.
Obtain Baseline Fasting Plasma Glucose Level: prior to initiation of potentially causative drugs, especially in patients with risk factors.
Low Dose and Short Duration: When a potentially offending drug is necessary, use at the lowest effective dose for the shortest duration of therapy, if possible.
Role of the Pharmacist
When pharmacists are aware of the potential medication-related problem of DI hypoglycemia and provide close monitoring and judicious use of the suspected drugs, adverse events can be prevented and/or minimized. Using resources to individualize therapy in older adults with comorbid conditions, anticipating patients’ questions about diabetes mellitus, and educating patients, their families, and caregivers about adherence and associated management and preventative measures are highly recommended.
REFERENCES
1. American Diabetes Association. Standards of medical care in diabetes—2017. Diabetes Care. 2017;40(suppl 1):S4-S135.
2. Seaquist ER, Anderson J, Childs B, et al. Hypoglycemia and diabetes: a report of a work group of the American Diabetes Association and the Endocrine Society. Diabetes Care. 2013;36:1384-1395.
3. Sease J. Diabetes mellitus. In: Chisholm-Burns MA, Schwinghammer TL, Malone PM, et al, eds. Pharmacotherapy: Principles & Practice, 5th ed. New York, NY: McGraw Hill Education; 2019:655-684.
4. Dang DK, Pucino Jr. F, Ponte CD, et al. Glucose and insulin dysregulation. In: Tisdale JE, Miller DA. Drug-Induced Diseases: Prevention, Detection, and Management, 3rd ed. American Society of Health-System Pharmacists, Inc. 2018:679-696.
5. Institute of Medicine. Envisioning the National Health Care Quality Report. Washington, DC: National Academies Press; 2001.
6. Shiyanbola OO, Farris KB. Concerns and beliefs about medicines and inappropriate medications: an internet-based survey on risk factors for self-reported adverse drug events among older adults. Am J Geriatr Pharmacother. 2010;8(3):245-257.
7. Stefanacci RG, Khan T. Can managed care manage polypharmacy? In: Zagaria MA. Polypharmacy. Clin Geriatr Med. 2017;33(2):241-255.
8. Lee JK, Mendoza DM, Mohler MJ, et al. Geriatrics. In: Chisholm-Burns MA, Schwinghammer TL, Malone PM, et al, eds. Pharmacotherapy: Principles & Practice, 5th ed. New York, NY: McGraw Hill Education; 2019:7-18.
9. Semla TP, Beizer JL, Higbee MD. Geriatric Dosage Handbook. 20th ed. Hudson, Ohio: Lexicomp; 2015:1193-1194.
10. Singh E, Vella A. Hypoglycemia after gastric bypass surgery. Diabetes Spectrum. 2012;25(4):217-221.
11. Whalen K, Sando KR. Diabetes mellitus MTM data set. In: Hardin HC, eds. Medication Therapy Management: A Comprehensive Approach. 2nd ed. New York, NY: McGraw Hill Education. 2018:343-363.
To comment on this article, contact rdavidson @uspharmacist.com.