US Pharm. 2020;45(9):22-26.
ABSTRACT: Infectious diseases are disorders caused by pathogenic microorganisms (e.g., bacteria, viruses, fungi, parasites) that may be transmitted directly or indirectly by various sources. Some infections may be harmful, but some may be harmless; all may be preventable. Certain patient populations may also be more susceptible to infections, including pregnant women. During pregnancy, some common infections that may occur are the flu, vaginal yeast infections, uterine infections, group B streptococcus, bacterial vaginosis, and listeria. Changes in immune function may cause this increased risk of infection, and if left untreated, may lead to serious complications. Complications from severe infections during pregnancy may include preterm birth, low birth weight, birth defects, learning problems, and possibly pregnancy loss. Prevention, early detection, and treatment are vital to help minimize and eliminate these complications.
Infectious diseases are disorders caused by pathogenic microorganisms (e.g., bacteria, viruses, fungi, parasites) that may be transmitted directly or indirectly by various sources (e.g., person to person, insects, animals, environment, food, water). Some infections may be harmful, but some may be harmless; all may be preventable. Certain patient populations, including pregnant women, may also be more susceptible to infections.1
During pregnancy, some common infections that may occur are influenza, vaginal yeast infections, eczema, herpes, uterine infections, group B streptococcus (GBS), bacterial vaginosis (BV), and listeria. Changes in immune function, such as reduction in T- and B-cell activity and natural killer–cell activity and increases in dendritic-cell activity, may cause this increased risk of infection.2,3 However, immune-system changes during pregnancy are not fully understood, and more data are needed.4
The severity of some infections, such as influenza, GBS, sexually transmitted diseases, urinary tract infections, and Zika virus, may also increase with advancing pregnancy.4 Complications from severe infections during pregnancy may include preterm birth, low birth weight, birth defects, learning problems, and possibly pregnancy loss.5-7 Prevention, early detection, and treatment are vital to help minimize and eliminate these complications with multiple available prevention and treatment strategies. The problem lies with growing and novel pathogens, as data are limited to devise a response plan to emerging infections such as the current pandemic.4,8
VIRAL VERSUS BACTERIAL
Many viral infections during pregnancy are considered benign; but due to the immunological changes that are associated with pregnancy, the severity of viral infections may increase.9 In addition, there is little available information about how pregnancy affects the mother’s response to viral pathogens; however, it is thought that placental response to viruses may play a role in the severity of infection.6,9 When pandemics such as influenza, Ebola, Zika, and COVID-19 occur, it becomes challenging to prevent and treat these infections with the complexity and uncertainty of immunological changes during pregnancy.9
Viruses and infections associated with pregnancy include herpes simplex virus (HSV); varicella zoster virus (also known as chickenpox); cytomegalovirus; rubella; human immunodeficiency virus (HIV); hepatitis; influenza; and Ebola.6
Bacterial infections may also affect women throughout their pregnancy term and the fetus and newborn. Like viral infections, it is just as important to screen, treat, and prevent these infections to decrease complications with pregnancy.10 Bacteria and infections associated with pregnancy include GBS; urinary tract infections; listeriosis; syphilis; chlamydia; and bacterial vaginosis.10
COMMON INFECTIONS AND TREATMENTS
Vaginal Infections: The most common vaginal infections are listed in TABLE 1. BV, which is an imbalance of the normal vaginal flora with an overgrowth of anaerobic bacteria, is the most commonly diagnosed vaginal infection. Women may be asymptomatic or report abnormal vaginal discharge and an unpleasant odor; however, infection can lead to premature labor unresponsive to tocolytic therapy.10 Identification and treatment may reduce the risk of preterm birth during pregnancy, and the recommended treatment for BV is oral or vaginal metronidazole or clindamycin; however, vaginal clindamycin cream is not recommended in the third or fourth trimester.10,11
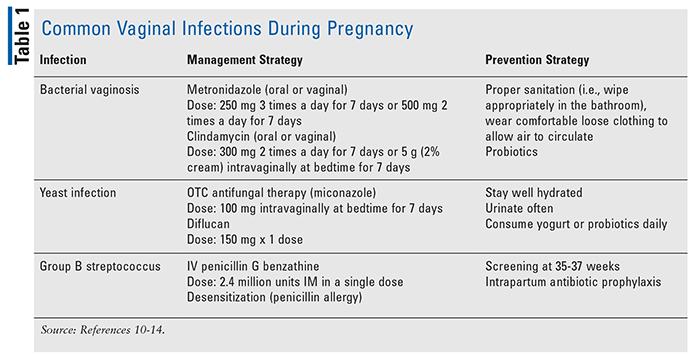
Yeast Infection or Vulvovaginal Candidiasis: This infection commonly occurs in pregnancy due to higher estrogen levels and glycogen content in vaginal secretions.12 Topical azole antifungals available OTC are recommended as first line with minimal risk of transfer to the fetus. A longer course of therapy of 7 days is preferred over a shorter duration.12 Oral fluconazole may be considered as second-line therapy; short-term use of 150 mg has not been shown to have an increased risk of malformations; however, case reports do show complications at higher doses above 400 mg.12,13
GBS: This is the most common cause of life-threatening infections in the newborn and possibly the mother. Infections that may occur include sepsis, pneumonia, or meningitis. Universal screening at 35 to 37 weeks of gestation, and intrapartum antibiotic prophylaxis are the key prevention strategies for GBS.14 If culture results are positive, treatment during labor is necessary with IV penicillin G (first-line preferred) or ampicillin (second-line option). Penicillin-allergic women may take clindamycin, vancomycin, or cefazolin as an alternative.14
RARER INFECTIONS AND TREATMENTS
Some rare infections may lead to serious complications. For example, primary HSV in pregnancy may lead to an increased risk of dissemination and hepatitis. Recurrence of HSV infection increases in frequency during pregnancy, which may lead to complications to the newborn post delivery.4 In addition, meta-analysis results show that prophylactic acyclovir beginning at 36 weeks’ gestation may reduce the risk of HSV recurrence at delivery, which may decrease risk of HSV viral shedding at delivery.15
When a pregnant woman infected with HIV goes into labor, the risk of transmitting HIV to the baby increases when the amniotic sac breaks. In order to protect the women’s health and also to prevent mother-to-child transmission, antiretroviral therapy against HIV infection is recommended.16 Guidelines recommend dolutegravir as the preferred antiretroviral therapy throughout pregnancy.16
Finally, syphilis in the fetus, left untreated, may cause severe complications such as stillbirth or deadly infection in the newborn. Screening is mandated early in pregnancy, and if tests are positive, treatment with penicillin G is the most effective therapy for prevention of transmission to the fetus.17 Pregnant women with a history of penicillin allergy are recommended to be desensitized and treated with penicillin as there are no preferred alternatives.17
URINARY TRACT INFECTIONS
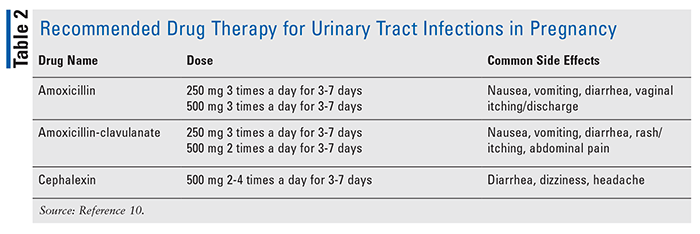
Asymptomatic urinary tract infections may occur in 10% to15% of pregnant women and can lead to complications, including premature labor.10 A urine culture is best to be completed as part of the screening process during early pregnancy to help treat the infection early and prevent complications, such as pyelonephritis.10 If a positive culture result exists, antibiotic therapy for 7 days is recommended to treat bacteriuria as shorter therapy is less effective. Amoxicillin, amoxicillin-clavulanate, and cephalexin are recommended therapies for urinary tract infections (TABLE 2); sulfonamides and nitrofurantoin are acceptable but have use limitations (i.e., sulfonamides are not recommended towards the end of pregnancy, and nitrofurantoin is not recommended in those with G6PD deficiency).
OTHER INFECTIONS
Besides vaginal and uterine infections, various other infections may occur during pregnancy that are important to note. (TABLE 3 also provides an overview of various other infections during pregnancy.)
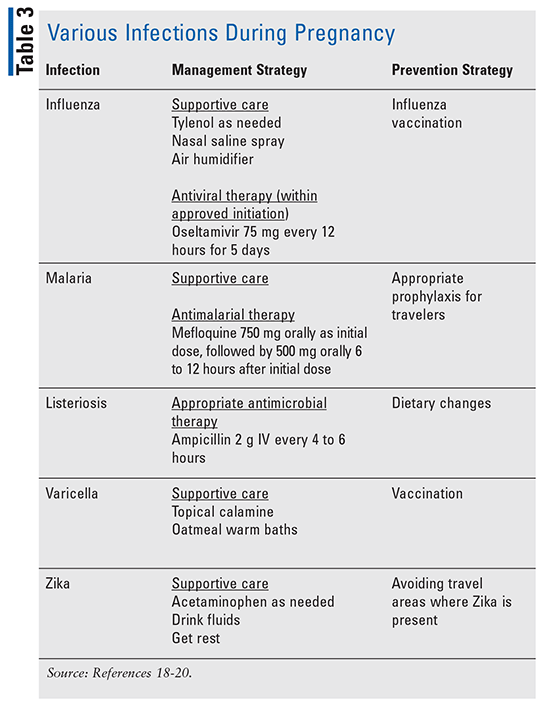
Influenza: Pregnant women may be at risk for severe illness from influenza virus infection. During the 2009 H1N1 influenza A pandemic, pregnant women were at an increased risk for severe disease leading to hospitalization or death; 5% of all deaths from the pandemic influenza were among pregnant women, who only represented 1% of the U.S. population at the time.18
Malaria: When malaria is left untreated, the infection can progress to severe complications. A study of three districts in India from 2004 to 2006 showed more than 23% of maternal deaths were due to malaria, which was the most common cause of maternal death in pregnancy at that time.19
Zika: Due to the outbreaks that occurred in 2016, recommendations on who receives testing for Zika havebeen updated. Testing is vital, as this infection may lead to severe complications, such as encephalopathy in newborns. Testing is recommended for symptomatic pregnant women who have traveled to areas with risk of Zika.20 Testing may be considered if a pregnant patient is asymptomatic but has traveled to areas with risk of Zika.20
COVID-19 CONSIDERATIONS DURING PREGNANCY
With the recent pandemic, the CDC has reviewed data and reports of COVID-19 results among pregnant women as part of COVID-19 surveillance.21 During January 22 to June 7, 2020, the CDC received reports of 326,335 women of reproductive age (15-44 years) who had positive test results for SARS-CoV-2, the virus that causes COVID-19; of these, 8,207 women were pregnant. Data show that pregnant women might be at increased risk for severe COVID-19 illness, such as respiratory illness. Symptomatic pregnant and nonpregnant women with COVID-19 reported similar frequencies of cough (>50%) and shortness of breath (30%), but pregnant women less frequently reported headache, muscle aches, fever, chills, and diarrhea. Among reproductive-age women with SARS-CoV-2 infection, pregnancy was associated with hospitalization and increased risk for ICU admission and receipt of mechanical ventilation, but not with death.21
To reduce COVID-19–associated illness, pregnant women should be aware of their potential risk for severe COVID-19 illness and prevention strategies that need to employed, such as not skipping prenatal care appointments, limiting interactions with other people as much as possible, and taking precautions to prevent becoming infected with COVID-19 when interacting with others.
TREATMENT BENEFITS VERSUS RISKS
Taking medications during pregnancy may be challenging and stressful for a woman. However, benefits versus risks must be reviewed prior to prescribing and dispensing. This may be challenging in many ways, as limited data are available to help support treatment when a pregnant woman may be asymptomatic, such as in BV, which can be present in up to 20% of women during pregnancy. BV may resolve without treatment if asymptomatic; however, it may develop into persistent infection later in pregnancy if untreated.11 One must also be careful with which medications have been shown to cause risk to the fetus, such as sulfonamides, trimethoprim, and nitrofurantoin.10,22 Reviewing available data and alternative therapies is needed to determine the best antibiotic therapy.
CONCLUSION
Infections during pregnancy are frequently benign; however, several and severe complications may occur if infections are left undetected or untreated. Monitoring for any signs and symptoms of infection during pregnancy is important, as well as following appropriate prevention and treatment strategies to help prevent the risk of complications in pregnancy and to the newborn.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
REFERENCES
1. Jamieson DJ, Theiler RN, Rasmussen SA. Emerging infections and pregnancy. Emerg Infect Dis. 2006;12(11):1638-1643.
2. Robinson DP, Klein SL. Pregnancy and pregnancy-associated hormones alter immune responses and disease pathogenesis. Horm Behav. 2012;62:263-271.
3. Pazos M, Sperling RS, Moran TM, Kraus TA. The influence of pregnancy on systemic immunity. Immunol Res. 2012;54:254-261.
4. Kourtis AP, Read JS, Jamieson DJ. Pregnancy and Infection. N Engl J Med. 2014;370(23):2211-2218.
5. Racicot K, Mor G. Risks associated with viral infections during pregnancy. J Clin Invest. 2017;127(15):1591-1599.
6. Silasi M, Cardenas I, Kwan JY, et al. Viral infections during pregnancy. Am J Reprod Immunol. 2015;73(3):199-213.
7. Medley N, Vogel JP, Care A, Alfirevic Z. Interventions during pregnancy to prevent preterm birth: an overview of Cochrane systematic reviews. Cochrane Database Syst Rev. 2018(11):CD012505.
8. Mei Y, Luo D, Wei S, et al. Obstetric management of COVID-19 in pregnant women. Front Microbiol. 2020;11:1186.
9. Racicot K, Mor G. Risks associated with viral infections during pregnancy. J Clin Invest. 2017;127(5):1591-1599.
10. Smith DS. Bacterial infections and pregnancy. Medscape. 2018. https://emedicine.medscape.com/article/235054-overview#a1. Accessed July 1, 2020.
11. McDonald HM, Brocklehurst P, Gordon A. Antibiotics for treating bacterial vaginosis in pregnancy. Cochrane Database Syst Rev. 2007(1):CD000262.
12. Soong D, Einarson A. Vaginal yeast infections during pregnancy. Can Fam Physician. 2009;55(3):255-256.
13. Norgaard M, Pedersen L, Gislum M, et al. Maternal use of fluconazole and risk of congenital malformations: a Danish population-based cohort study. J Antimicrob Chemother. 2008;62(1):172-176.
14. American College of Obstetricians and Gynecologists Committee on Obstetric Practice. ACOG Committee Opinion No. 485: Prevention of early-onset group B streptococcal disease in newborns. Obstet Gynecol. 2011;117(4):1019-1027.
15. Sheffield JS, Hollier LM, Hill JB, et al. Acyclovir prophylaxis to prevent herpes simplex virus recurrence at delivery: a systematic review. Obstet Gynecol. 2003;102(6):1396-1403.
16. HHS Panel on Treatment of Pregnant Women with HIV Infection and Prevention of Perinatal Transmission. Recommendations for the use of antiretroviral drugs in pregnant women with HIV infection and interventions to reduce perinatal HIV transmission in the United States. http://aidsinfo.nih.gov/contentfiles/lvguidelines/perinatalgl.pdf. Accessed July 1, 2020.
17. Workowski KA, Bolan GA. Sexually transmitted diseases treatment guidelines, 2015. MMWR Recomm Rep. 2015;64(RR-03):1-137.
18. Siston AM, Rasmussen SA, Honein MA, et al. Pandemic 2009 influenza A(H1N1) virus illness among pregnant women in the United States. JAMA. 2010;303(15):1517-1525.
19. Rijken MJ, McGready R, Boel ME, et al. Malaria in pregnancy in the Asia-Pacific region. Lancet Infect Dis. 2012;12(1):75-88.
20. Sharp TM, Fischer M, Munoz-Jordan JL, et al. Dengue and Zika virus diagnostic testing for patients with a clinically compatible illness and risk for infection with both viruses. MMWR Recomm Rep. June 14, 2019;68(1):1-10.
21. Ellington S, Strid P, Tang VT, et al. Characteristics of women of reproductive age with laboratory-confirmed SARS-CoV-2 infection by pregnancy status–United States, January 22-June 7, 2020. MMWR Morb Mortal Wkly Rep. 2020;69:769-775. /
22. Crider KS, Cleves MA, Reefhuis J, et al. Antibacterial medication use during pregnancy and risk of birth defects: National Birth Defects Prevention Study. Arch Pediatr Adolesc Med. 2009;163(11):978-985.
To comment on this article, contact rdavidson@uspharmacist.com.






