US Pharm. 2021;46(6):4-9.
ABSTRACT: Urinary incontinence (UI) is an involuntary leakage of urine, and various types of male UI differ in their etiologies, clinical manifestations, and treatments. While working with patients, pharmacists should be aware that men may be reluctant to bring incontinence to the attention of their clinician. The work-up of transient UI typically involves identifying possible reversible causes and often implicates drug classes that impair urine flow, bladder contractions, or cognition. Adjunctive and nonpharmacologic care may be used initially, but more severe symptoms require medications and/or surgery, depending on the patient’s preference and predominating symptomology.
Urinary incontinence (UI) is the loss of bladder control. It affects many men and impacts their quality of life.1 One in five men with symptoms of UI were likely to seek care, and men were only half as likely as women to seek care (22% vs. 45%, respectively).2,3 Pharmacists are in ideal positions to engage with male patients about their health and wellbeing. They can discuss medications and provide guidance on an earlier referral.
Without early recognition, UI can limit participation in activities and reduce quality of life. Men with UI have higher rates of depression and are more likely to decrease participation in their work life (e.g., changing employment, retiring earlier). Moreover, UI may even have a greater emotional and social impact on quality of life for men than for women.4-6 Men are also more likely to experience UI with increasing age. In some studies, the prevalence of UI in men older than age 65 years ranged from 11% to 34%, with a prevalence of daily incontinence of 2% to 11%.6 The prevalence in men living in nursing homes is higher compared with community settings, and men with UI have a higher risk of institutionalization. Inpatient pharmacists should be especially aware of this to help assess the impact and safety of medical interventions for these patients.2,3,7,8 Among community-dwelling men, one study also demonstrated increasing prevalence with age, finding that among men with at least one UI episode in the preceding 12 months, prevalence increased from almost 5% at ages 19 to 44 years to 11.2% at ages 45 to 64 years, and to 21% in men older than age 65 years.9
CLASSIFICATION
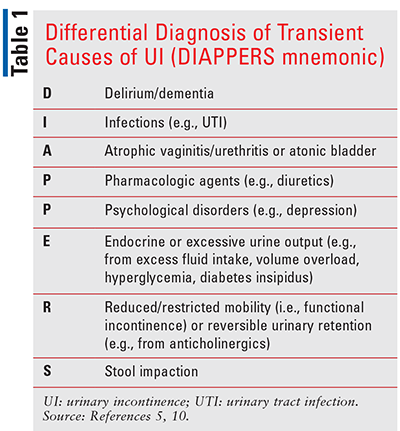
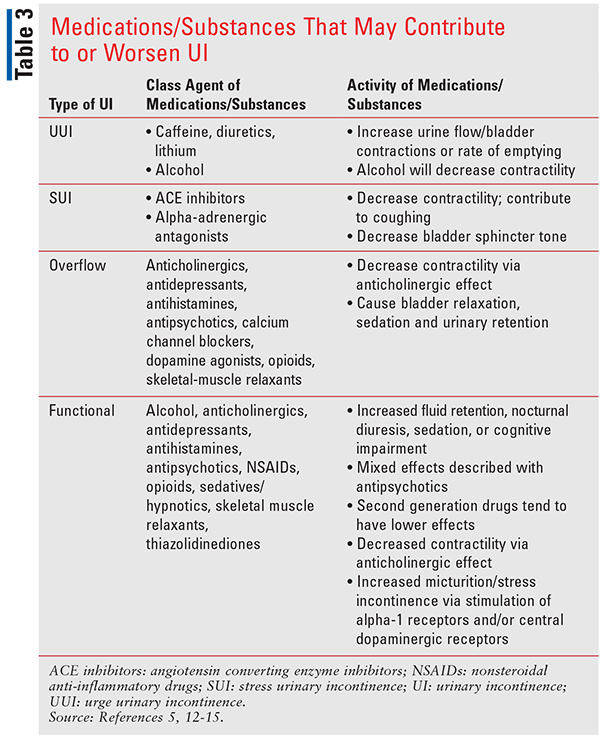
Types of male UI differ in their etiologies, clinical manifestations, and treatments. Generally, the first step in the diagnostic evaluation of a patient presenting with UI is to determine whether the symptoms are transient/reversible or chronic. Pharmacists can play a role in reviewing/assessing risk factors for UI (using the DIAPPERS mnemonic), as well as the patient’s medications to determine if the UI is transient/reversible UI (TABLE 1). Pharmacists can help providers identify possible drugs or substances that may worsen each type. It is worth noting that patients may present with more than one type of UI. The etiology of each type of incontinence may be multifactorial, with a variety of contributing pathophysiologic mechanisms (TABLE 2). In particular, pharmacists can assist with patients in nursing homes or hospitals, where polypharmacy increases the risk of adverse events (TABLE 3).1, 5,6,10,11
GENERAL MANAGEMENT
Regardless of the type of UI, discussing the patient’s goals and expectations of treatment is key. A multicomponent approach focused on aspects of UI that are most bothersome to the patient is important for successful management. Treatment aimed at simply decreasing the number of incontinence episodes may not be enough to improve quality of life for patients who are most bothered by the timing, volume, or inconvenience of UI. For some men, a period of continence sufficient to complete an activity (e.g., work meeting, car ride, or attending an event) is a major goal; for other men, avoiding side effects from medications (where a pharmacist can assist) or a surgical procedure is more important.
Adjunctive Measures
During evaluation and initiation of treatment, pharmacists should be aware that men with any type of incontinence may be using adjunctive measures (e.g., protective pads, external catheters). Male patients should be informed that leakage is not a normal part of aging and that goals of treatment include minimizing or eliminating the need for pads or catheters as a self-management strategy. Although some men may continue to use these measures over the long term as well, these should not be the only treatments, because chronic use is associated with certain risks. Adding treatments to correct the underlying cause(s) of incontinence may decrease the need for adjunctive measures and mitigate associated risks. Pharmacists can play a role in counseling patients on the risks of chronic or frequent use of pads (e.g., infections, contact dermatitis), which can be minimized by ensuring regular changes of pads or garments when leakage occurs.16
Nonpharmacologic Treatment
Nonpharmacologic therapies for urge UI (UUI), stress (SUI), and mixed incontinence include16:
• Pelvic-floor muscle exercises, using the same techniques for men and for women
• Lifestyle changes (e.g., weight loss, fluid consumption)
• Bladder training (e.g., scheduled voiding, based on a voiding diary)
• Biofeedback
MANAGING SPECIFIC TYPES OF UI
Stress Urinary Incontinence
Nonpharmacologic Therapy: Nonpharmacologic therapy is generally used for initial management of SUI along with adjunctive measures. In systematic reviews, meta-analyses, and randomized trials, results differ as to whether there is benefit of nonpharmacologic therapies for postsurgical UI. For some men with SUI, a penile clamp to mechanically hinder involuntary passage of urine may be used intermittently.17
Pharmacotherapy: For men with SUI who do not respond to lifestyle interventions or pelvic-floor muscle exercises after a few months, pharmacists may see duloxetine, a serotonin norepinephrine reuptake inhibitor, added on. Duloxetine is approved for the treatment of SUI in many European countries. However, in the United States, there are no medications approved for SUI (i.e., duloxetine is approved to treat major depression and neuropathic pain). The thought of using duloxetine is that it acts by stimulating pudendal motor neuron alpha-adrenergic and 5-hydroxytryptamine-2 receptors, which can improve urinary symptoms. A systematic review found limited evidence to support the efficacy of any single medication for male UI, except for one well-performed randomized trial. In this trial of 112 men with postprostatectomy SUI, after 16-week follow-up those randomly assigned to duloxetine along with pelvic-muscle exercises were more likely to report improved incontinence-related quality of life compared with those assigned to pelvic-muscle exercises alone, and 39 (vs. 27) patients were dry. Pharmacists should set expectations with their patients as the beneficial effect of duloxetine quickly disappeared after discontinuation in the study. Additionally, it would be important to share the side-effect profile of nausea and ways to manage it while on treatment as patients were more likely to discontinue duloxetine compared with placebo (15% vs. 2%) during the study period, with nausea being the most common reason.18
Procedural and Surgical Interventions: The most common interventions for male SUI are transurethral bulking agents, perineal slings, and an artificial urinary sphincter (TABLE 4), which are coordinated by urologists. For men experiencing incontinence following radical prostatectomy, watchful waiting supplemented with nonpharmacologic therapy for a period of at least 6 to 12 months is generally recommended (as the SUI symptoms may resolve on their own). Selecting among these therapies depends upon the severity of the incontinence and whether the patient is healthy enough to undergo one of the surgical procedures. For men who choose to have surgery for SUI, the main treatment decision is between surgical placement of a perineal sling and an artificial urinary sphincter. The choice is based on patient preference.16

Urge Urinary Incontinence
For men with UUI, nonpharmacologic therapy is typically used for initial management along with adjunctive measures. If symptoms persist, pharmacotherapy is added, and procedural or surgical treatment is an option for incontinence refractory to pharmacotherapy. According to the American Urological Association/Society of Urodynamics, Female Pelvic Medicine & Urological Reconstruction guidelines, anticholinergics are recommended as second-line treatment; however, they are associated with an increased risk of developing possibly irreversible dementia in older adults. Pharmacists may want to be proactive in discussing the risk-benefit ratio of chronic anticholinergic treatment with both the healthcare practitioner and patients, especially those older than age 75 years or at risk for dementia. An alternative treatment for UUI associated with overactive bladder (OAB) could be a beta-3 adrenergic agonist (mirabegron), which is not associated with dementia and is a better option for elderly patients. However, this agent may have a financial burden for patients and discussing other alternative dose or route strategies can sometimes help with the side effects of anticholinergics. From the patients,’ perspective, patient-reported outcomes in OAB symptoms are equivalent among antimuscarinics (e.g., darifenacin, fesoterodine, oxybutynin, solifenacin, tolterodine, trospium) and mirabegron. However, it is important to be mindful of limiting the use of anticholinergics in those patients on acetylcholinesterase inhibitors due to their opposing mechanism-of-action effects.13,19,20
For men with symptoms suggestive of bladder outlet obstruction (BOO), studies support using combination treatment of an alpha blocker (e.g., alfuzosin, doxazosin, silodosin, tamsulosin, terazosin) and a phosphodiesterase type 5 inhibitor (e.g., tadalafil).21,22
For men with both BOO and OAB symptoms, treatment can be more challenging. A systemic review showed that initiating alpha-blocker treatment first and then adding an antimuscarinic treatment secondarily appears to be the most appropriate approach when considering both safety and efficacy. In men with BOO and OAB symptoms and where cognition is of concern, it has been shown that a combination of tamsulosin and mirabegron is both safe and efficacious.21-23
Mixed Incontinence
In men with mixed incontinence, a combination of treatment for SUI and UUI is indicated. Treatment should be individualized according to the etiologies and the relative severity of the UUI versus the SUI. Generally, the type of incontinence that started more recently is treated first, followed by symptom reassessment.5
Postvoid Dribbling
A man with retained urine in the urethra causing post-void dribbling should be advised to avoid compression of the urethra during voiding, such as from undergarments or pants. They are usually counseled, following micturition, to manually “milk” the perineal urethra to expel retained urine. Pelvic-floor exercises may also be used. However, there is no direct evidence of efficacy with these interventions.5
MEASURING TREATMENT EFFECTIVENESS
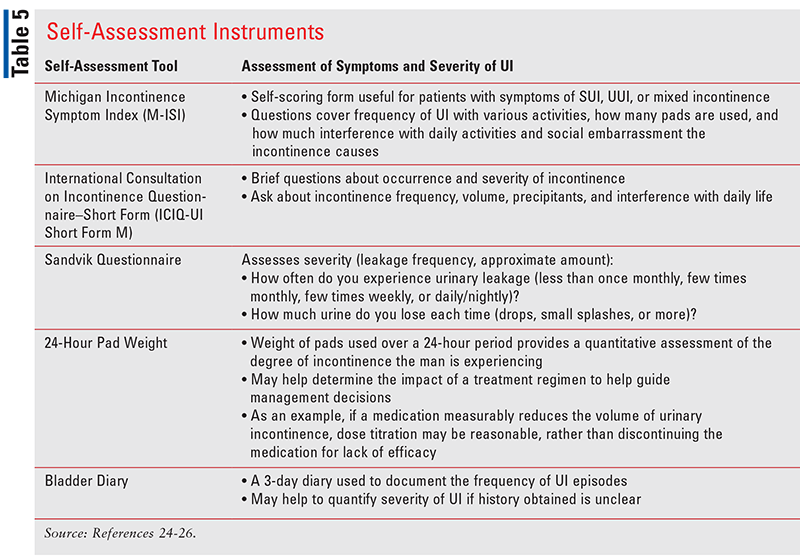
Self-assessment instruments for UI may be used to measure patient-reported outcomes. Additionally, comparing results during or after treatment with those obtained during initial evaluation of incontinence may help the patient and clinician assess treatment effectiveness (TABLE 5).24-26
CONCLUSION
Urinary incontinence in men may be debilitating, and men may not bring up their symptoms to their physician. Pharmacists could aim discussions at identifying men who are experiencing UI and need further evaluation. First-line treatments for UI are generally adjunctive and nonpharmacologic, whereas medications and surgery are reserved for patients who are refractory to these measures, have more severe symptoms, and/or prefer this route of treatment. Pharmacists can play a role in the continuous monitoring of the effectiveness and tolerability of the agents prescribed, and they can provide valuable instruction, intervention, and recommendations to improve patient outcomes in the management of UI.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
REFERENCES
1. D’Ancona CD, Haylen B, Oelke M, et al. An International Continence Society (ICS) report on the terminology for adult male lower urinary tract and pelvic floor symptoms and dysfunction. Neurourol Urodyn. 2019;38(2):433-477.
2. Tennstedt SL, Chiu GR, Link CL, et al. The effects of severity of urine leakage on quality of life in Hispanic, white, and black men and women: the Boston community health survey. Urology. 2010;75(1):27-33.
3. Harris SS, Link CL, Tennstedt SL, et al. Care seeking and treatment for urinary incontinence in a diverse population. J Urol. 2007;177(2):680-684.
4. Lagro-Janssen TALM, Hilkens CJM, Klaasen RI, Teunissen D. Greater emotional and social effect of urinary incontinence in men than women. J Am Geriatr Soc. 2008;56(9):1779-1781.
5. Khandelwal C, Kistler C. Diagnosis of urinary incontinence. Am Fam Physician. 2013;87:543-550.
6. Litwin MS, Saigal CS, eds. Urologic Diseases in America. Urinary incontinence. U.S. Department of Health and Human Services, Public Health Service, National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases. Washington, DC: U.S. Government Printing Office; 2012:97-160. NIH Publication No. 12-7865.
7. Sahyoun NR, Pratt LA, Lentzner H, et al. The changing profile of nursing home residents: 1985-1997. Aging Trends. 2001;(4):1-8.
8. Baztán JJ, Arias E, Gonzalez N, Rodriguez de Prada MI. New-onset urinary incontinence and rehabilitation outcomes in frail older patients. Age Ageing. 2005;34(2):172-175.
9. Shamliyan TA, Wyman JF, Ping R, et al. Male urinary incontinence: prevalence, risk factors, and preventive interventions. Rev Urol. 2009;11(3):145-165.
10. Erdem N, Chu FM. Management of overactive bladder and urge urinary incontinence in the elderly patient. Am J Med. 2006;119(3 suppl 1):29-36.
11. Lucas MG, Bosch RJL, Buckhard FC, et al. EAU guidelines on assessment and nonsurgical management of urinary incontinence. Eur Urol. 2012;62:1130-1142.
12. Curtis LA, Dolan TS, Cespedes RD. Acute urinary retention and urinary incontinence. Emerg Med Clin North Am. 2001;19:591-619.
13. Gormley EA, Lightner DJ, Burgio KL, et al. Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. J Urol. 2012;188 (suppl 6):2455-2463.
14. Verhamme KMC, Sturkenboom MCJM, Stricker BHC, Bosch R. Drug-induced urinary retention. Drug Saf. 2008;31:373.
15. Zyczynski H, Parekh M, Kahn MA, Rardin C. Urinary incontinence in women. American Urogynecologic Society (2012). http://eguideline.guidelinecentral.com/i/76622-augs-urinary-incontinence. Accessed May 19, 2021.
16. DeMaagd GA, Davenport TC. Management of urinary incontinence. PT. 2012;37(6):345-361.
17. Shamliya TA, Wyman JF, Ping R, et al. Male urinary incontinence: prevalence, risk factors, and preventive interventions. Rev Urol. 2009;11(3):145-165.
18. Filocamo MT, Marzi VL, Popola GD, et al. Pharmacologic treatment in postprostatectomy stress urinary incontinence. Eur Urol. 2007;51(6):1559-1569.
19. American Geriatrics Society Beers Criteria Update Expert Panel. American Geriatrics Society 2015 updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults. J Am Geriatr Soc. 2015;63:2227-2246.
20. Gray SL, Anderson ML, Dublin S, et al. Cumulative use of strong anticholinergics and incident dementia: a prospective cohort study. JAMA Intern Med. 2015;175:401-407.
21. Regadas RP, Reges R, Cerqueira JBG, et al. Urodynamic effects of the combination of tamsulosin and daily tadalafil in men with lower urinary tract symptoms secondary to benign prostatic hyperplasia: a randomized, placebo-controlled clinical trial. Int Urol Nephrol. 2013;45(1):39-43.42.
22. Athanasopoulos A, Chapple C, Fowler C, et al. The role of antimuscarinics in the management of men with symptoms of overactive bladder associated with concomitant bladder outlet obstruction: an update. Eur Urol. 2011;60(1):94-105.
23. Ichihara K, Masumori N, Fukuta F, et al. A randomized controlled study of the efficacy of tamsulosin monotherapy and its combination with mirabegron for overactive bladder induced by benign prostatic obstruction. J Urol. 2015;193(3):921-926.
24. Twiss CO, Fischer MC, Nitti VW. Comparison between reduction in 24-hour pad weight, International Consultation on Incontinence-Short Form (ICIQ-SF) score, International Prostate Symptom Score (IPSS), and Post-Operative Patient Global Impression of Improvement (PGI-I) score in patient evaluation after male perineal sling. Neurourol Urodyn. 2007;26(1):8-13.
25. Suskind AM, Dunn RL, Morgan DM, et al. The Michigan Incontinence Symptom Index (M-ISI): a clinical measure for type, severity, and bother related to urinary incontinence. Neurourol Urodyn 2014;33:1128-1134.
26. Sandvik H, Espuna M, and Hunskaar S. Validity of the incontinence severity index: comparison with pad-weighing tests. Int Urogynecol J Pelvic Floor Dysfunct 2006;17:520-524.
To comment on this article, contact rdavidson@uspharmacist.com.