US Pharm. 2022;47(5):HS6-HS12.
ABSTRACT: The prevalence of electronic cigarette (EC) use, or vaping, by U.S. adults and adolescents is rising. Some perceived advantages of ECs include flavor variety, accessibility, lower cost, and health benefits over combustible cigarettes (CCs). Although they are not FDA approved, ECs are considered an effective smoking-cessation aid. Similar to CCs, the pathophysiology of EC-induced neurodysregulation (stroke and seizure) involves oxidative stress–mediated neuroinflammation and impairment of the blood-brain barrier. Pharmacists should acquire a deeper understanding of the varying EC-device formulations in order to best counsel patients on the potential adverse health risks as well as the benefits for smoking cessation.
Electronic cigarettes (ECs) first emerged on the consumer market in 2003. Originally intended as a safer alternative to conventional combustible cigarettes (CCs), vaping has become popular among adults and adolescents.1 More than 5.6 million U.S. adults currently vape, with more than 2.2 million of those being current CC smokers, more than 2.1 million being former smokers, and more than 1.3 million being never-smokers.2 Vaping prevalence is highest among men; non-Hispanic white, American Indian/Alaskan Native, and multiracial populations; and individuals with a higher education level (excluding those with a college degree).2 Alarmingly, 63.4% of never-smokers who vape are young: ages 18 to 24 years.2
Epidemiologic data indicate that vaping is on the rise, with the majority of adult CC smokers turning to ECs to reduce their health risk; to aid in smoking cessation (i.e., alternative nicotine delivery); or to supplement conventional CC use based on convenience or consideration of others.3,4 On average, EC users vape the equivalent of approximately 15 cigarettes per day.5 ECs are not currently FDA approved for smoking cessation, and they may have detrimental effects.6-9 Although CC smoking among U.S. adolescents is on the decline, EC use has increased. Between 2017 and 2019, EC use increased from 11.7% to 27.5% in high school students and from 3.3% to 10.5% in middle school students.10-12 Also, concern is growing that vaping may serve as a gateway to CC smoking, especially in youths.13-16
Whereas adolescents are more likely to use ECs because of social pressure, adults are more likely to use them as a CC replacement based on perceived health benefits, such as improved breathing and reduced symptoms of chronic obstructive pulmonary disease and asthma.1,17,18 In fact, patients who switched from CCs to ECs showed significant improvements in carboxyhemoglobin and oxygen-saturation levels after just 2 weeks.19 Other perceived advantages of ECs include flavor variety, ease of access, belief that they may be used both indoors and outdoors since they do not have a strong tobacco smell, and lower cost. (In fact, cost analyses demonstrate a savings of $1,500 to $2,000 per year with the use of ECs compared with consumption of one pack of CCs per day.20) Many EC users believe that the vapor from ECs is not harmful to others.18 CC smokers’ reasons for vaping often differ from those of non-users; for example, a survey of CC smokers and nonusers determined that limiting flavor options would deter nonusers from vaping but would not impact CC smokers.21
Neurologic dysfunction—which manifests as cerebrovascular dysfunction (stroke, seizure), neuroinflammation, nicotine addiction, and behavioral and mental health problems (impaired short-term memory, concentration, learning, and self-control/attention as well as anxiety and other mood disorders)—is emerging as a potential adverse effect of vaping.22-28 This article will present the pathophysiology of EC-induced neurodysfunction, discuss therapeutic options, and highlight the role of the pharmacist in counseling patients on the health benefits versus risks of vaping.
EC DEVICES
Despite a lack of conclusive safety data, the general public perception that ECs are a healthier alternative to CCs motivates many individuals to vape.3,4,29 This belief stems largely from the fact that EC devices produce an aerosol that delivers inhalable nicotine without generating carbon monoxide and other harmful toxicants that are widely known to cause serious adverse pulmonary and cardiovascular problems.30 EC devices consist of a heating element, battery, and cartridge filled with an e-liquid solution containing the solvent carriers propylene glycol (PG) and/or vegetable glycerin (VG), nicotine, and flavorings.31-33 Although their long-term toxicity remains relatively unknown, a growing body of evidence suggests that ECs may cause acute cardiopulmonary damage.22,34,35 EC-induced toxicity varies considerably based on device design (e.g., voltage, temperature, automated vs. manual aerosol production).36 Variations in physical factors such as e-liquid composition, heating-coil temperature, and puffing topography (e.g., volume) can influence vapor production, degree of nicotine and other EC-component intake, and extent of toxicity.37 Moreover, several toxic or carcinogenic chemicals strongly implicated in cardiopulmonary disease have been identified in components of ECs.38
PATHOPHYSIOLOGY OF EC-INDUCED NEUROTOXICITY
Although research on the mechanisms underlying EC-induced neurotoxicity is limited, impaired integrity of the blood-brain barrier (BBB) appears to be a key factor.39-42 The BBB, a selective permeability barrier formed by tight junctions between endothelial cells, acts as the protective gatekeeper for the passage of solutes into and out of the brain. The antioxidant signaling molecule nuclear factor erythroid 2-related factor (Nrf2) regulates the expression of endothelial tight junction proteins that maintain BBB integrity and restrict permeability.43-46 Oxidative stress and neuroinflammation lead to the breakdown of this critical barrier. Reactive oxygen species (ROS), which are endogenously generated in the mitochondria during normal cellular processes, can be introduced into the body when the vaporized chemical constituents of ECs are inhaled.36,47 Excessive ROS production can overwhelm built-in antioxidant defense systems, resulting in oxidative stress and neuroinflammation.
Multiple lines of evidence have identified the BBB as a major link between CCs and neurodysfunction.48 It is well established that CCs induce oxidative stress–driven vascular endothelial dysfunction mediated by nicotine and ROS.49-53 Nicotine also dysregulates ions and glucose transporters (GLUT1 and GLUT3) in cerebral microvessels and increases BBB permeability, in part by reducing the expression of—and adversely altering—the cellular distribution of several tight junction proteins.41,54,55 EC vapor extracts compromise BBB integrity via similar mechanisms.43,46,56,57 Like CCs, they disrupt the cellular antioxidant response system by downregulating Nrf2 expression, increasing permeability, and reducing or altering the cellular-distribution pattern of tight junction proteins.39,46,57 Also, the activity of the pro-oxidant enzyme NADPH oxidase 2 and the oxidative stress marker peroxisome proliferator-activated receptor is upregulated.46,57,58 Both CCs and ECs disrupt mitochondrial membrane potential (i.e., elicit depolarization) in brain microvascular endothelial cells in mice and dysregulate cellular iron and redox homeostasis.40
Neuroinflammation involves the interplay between immune cells, cytokines, adhesion molecules, and matrix metalloproteinases, resulting in cellular damage that can compromise BBB integrity and cerebral vasculature.59 Preclinical data show that vascular markers of inflammation are upregulated in murine brain and human plasma in response to EC vapor exposure.27,36,46,59,60 Moreover, stroke injury is greater in mice that were chronically exposed to EC vapor than in mice that were not.46 Users of ECs demonstrate increased levels of inflammatory biomarkers compared with levels in nonusers.59 Although data are limited, these adverse cellular and molecular events implicate vaping-induced toxicity at the BBB as a mechanism by which EC vapor could cause or exacerbate neurodysfunction.
NEURODYSFUNCTION ASSOCIATED WITH ECs
Given that vaping is a relatively new practice, there is a paucity of information about potential adverse impacts on health. Oxidative stress–mediated BBB disruption is strongly implicated in several neurologic diseases, including ischemic stroke, Alzheimer’s disease (AD), traumatic brain injury, and Parkinson’s disease (PD).60 Moreover, tobacco smoke is strongly associated with increased risk of stroke, AD, multiple sclerosis, and vascular dementia.40,61 In epileptic patients, EC use increases the frequency of seizures.62 Oxidative stress and neuroinflammation are involved in the etiology and pathogenesis of ischemic stroke and PD, respectively. BBB damage caused by EC use may worsen outcomes in these neurologic conditions, as evidenced by increased infarct size following EC exposure in a murine ischemic stroke model.46
Stroke
The brain is a principal user of glucose in the body, and nicotine reduces glucose transport at GLUT1 and GLUT3 receptors located in the BBB. With ischemic stroke, the impacted brain region is deprived of blood flow, reducing the delivery of glucose and oxygen; however, the impact on glucose utilization remains unclear.41 Although ECs may worsen ischemic stroke injury via impaired glucose handling, no definitive evidence exists that they contribute to its etiology.41,63 The pathophysiology of stroke is multifactorial and includes the development of atherosclerosis and coagulopathy resulting from various causes.63 In current smokers, a prolonged EC smoking session (i.e., 30 minutes) had similar effects on blood pressure and aortic stiffening compared with CC-using counterparts.64,65 Therefore, it could be hypothesized that EC use increases stroke risk.64
Few studies have examined specific effects of EC use in stroke pathogenesis, and results are inconclusive. In one study, transient alterations in endothelial and microvascular function occurred with the use of nicotine-free ECs in healthy nonsmokers.66 In a separate study comparing nonsmokers, CC users, and EC users, there was no increased stroke risk in EC users versus nonsmokers, and the stroke risk was reduced in EC users versus CC users.63,67 CC users and dual users (i.e., both CCs and ECs) exhibited worsened hemodynamic effects compared with nonusers and sole-EC users, as evidenced by differences in blood pressure and pulse-wave variation.68
Seizure
ECs contain a mixture of concentrated nicotine, PG, VG, and/or additional substances for flavoring and solubility. These substances can affect or result in seizure activity.
Nicotine: Case reports describe instances of nicotine intoxication from EC liquid, ranging from unintentional ingestions in young children to intentional suicide attempts in adults.69 In patients with nicotine levels at supralethal doses, the most common symptoms are tachycardia, altered mental status, and vomiting. In general, however, a wide variety of symptoms are associated with nicotine toxicity, which may be partly explained by the systemic distribution of cholinergic nicotinic receptors. Nicotine not only functions systemically at the neuromuscular junction but can also directly affect the central nervous system. Nicotine is thought to involve desensitization of central cholinergic receptors at extremely high doses. These receptors would typically stimulate gamma-aminobutyric acid (GABA)ergic activity to inhibit pyramidal neurons. Upon desensitization and downregulation, GABAergic activity is reduced, resulting in pyramidal neuron excitation and seizure.69 Seizures stemming from nicotine intoxication are most likely to occur during or soon after EC use, as this is when systemic nicotine concentration is highest.25 Patients are likely to experience other systemic effects of nicotine toxicity during this period.
PG: The FDA has designated this solvent commonly used in medications, foods, and cosmetics as Generally Regarded as Safe (GRAS).69,70 However, the GRAS classification does not apply to inhalation products.23 PG can be toxic at very high doses, particularly if given over a short time. Although the World Health Organization has recognized a maximum consumption level, there is no maximum recommended dose for pharmaceutical preparations or ECs.71 PG is metabolized mostly in the liver and is converted to water and carbon dioxide through the citric acid cycle, with less than 50% eliminated unchanged by the kidney. In patients with low levels of alcohol dehydrogenase or kidney disease, the potential for accumulation and toxicity is increased. PG toxicity manifests as hyperosmolar metabolic acidosis that may lead to seizure.69,71 The amount of PG by-products (acrolein, formaldehyde) found in ECs is much lower than in CCs and is not linked to acute seizure induction.25
VG: VG has not been extensively studied as an EC additive. Like PG, it is used in food products because of its sweet taste and favorable safety profile, and it is classified as GRAS for oral consumption. VG undergoes hepatic metabolism and ultimately enters the citric acid cycle, where it is esterified with fatty acids and is eliminated renally.69,70 Owing to its osmotic properties, VG may induce dehydration, which could potentiate seizure activity if the dehydration is sufficiently severe.69
Additional Substances: Other constituents used legally in EC vapor devices, such as ethanol, tetrahydrocannabidiol, and cannabidiol, are not linked to seizure activity.23 However, reports of adulterated products containing seizure-inducing synthetic substances have surfaced, making it critically important to examine the contents of users’ products.25
Anxiety and Mood Disorders
Both EC use and nicotine use negatively impact anxiety, depression, concentration, and learning, particularly among adolescents, whose brains are still developing.72,73 The younger an individual is at first use, the greater the risk of nicotine addiction.72 Nicotine increases the release of the neurotransmitter dopamine, stimulating the brain’s reward circuitry to reinforce the effects of nicotine and cause addiction. Depression is typically correlated with low dopamine levels. Compared with nonsmokers, smokers with depression experience elevated dopamine release, which heightens the reinforcing effects of smoking.74 Nicotine withdrawal can also lead to negative emotions and effects such as anxiety, increased stress, difficulty concentrating, depressed mood, irritability, increased appetite, insomnia, and tobacco cravings. One explanation for these effects is the decrease in dopamine release after quitting smoking that can occur long after cessation.75 Former smokers are less likely than current smokers to experience depression; however, this is not true for current EC users.76,77 Former EC users have a 1.6 times higher rate of history of depression than non-users, and current EC users have an even higher rate (2.1 times higher).78
THE PHARMACIST’S ROLE
Pharmacists have the opportunity to become frontline leaders in educating patients on EC use. This requires a deeper understanding of how EC devices work, the advantages and disadvantages of EC use, and public perceptions about the safety and efficacy of ECs as a smoking-cessation tool. Pharmacists are faced with the challenge of recommending ECs as a smoking-cessation aid while supplying information about the potential risks. Working knowledge of the causal links between EC use and neurologic dysfunction, therefore, is critical to providing accurate, evidence-based information to patients considering using these devices. TABLE 1 highlights the positive and negative attributes of ECs, which can help patients weigh the advantages and disadvantages.79-81

Many of the adverse neurologic effects of ECs are the same as those of CCs. Both types of products impair BBB integrity, elicit neuroinflammation, and exacerbate stroke injury.39,41,42,46 Therefore, complications arising from EC-induced neurodysfunction are treated in a manner similar to those arising from CC use. Dual users are at greater risk for heart disease, lung disease, and cancer.82 Preclinical studies posit new indications for drugs that are routinely used for other conditions. The antidiabetic agents metformin and rosiglitazone prevent both EC vapor–induced oxidative stress and BBB impairments.39,43,46,57 These agents restore healthy redox homeostasis by abrogating EC-induced decreases in Nrf2 and tight junction proteins, and they reduce vascular inflammation.39,43,46,57
CC smokers aged 18 years and older have used nicotine replacement therapy (NRT), bupropion, varenicline, and behavioral counseling for smoking cessation. Although ECs are not FDA approved, they are touted as an alternative smoking-cessation tool. Because ECs are still relatively new, limited evidence-based data exist on the use of ECs as a strategy for CC smoking cessation and on strategies for vaping cessation. Because many EC products contain nicotine, healthcare providers have treated vaping cessation similarly to CC smoking cessation.83 Several clinical trials have shed light on the effectiveness of ECs in helping CC smokers quit. Notably, CC smokers perceive ECs to be more satisfying than nicotine inhalers.84 Given this perception, a patient could perhaps be switched from CCs to a nicotine-containing EC, with the nicotine concentration deescalated over time to avoid withdrawal.
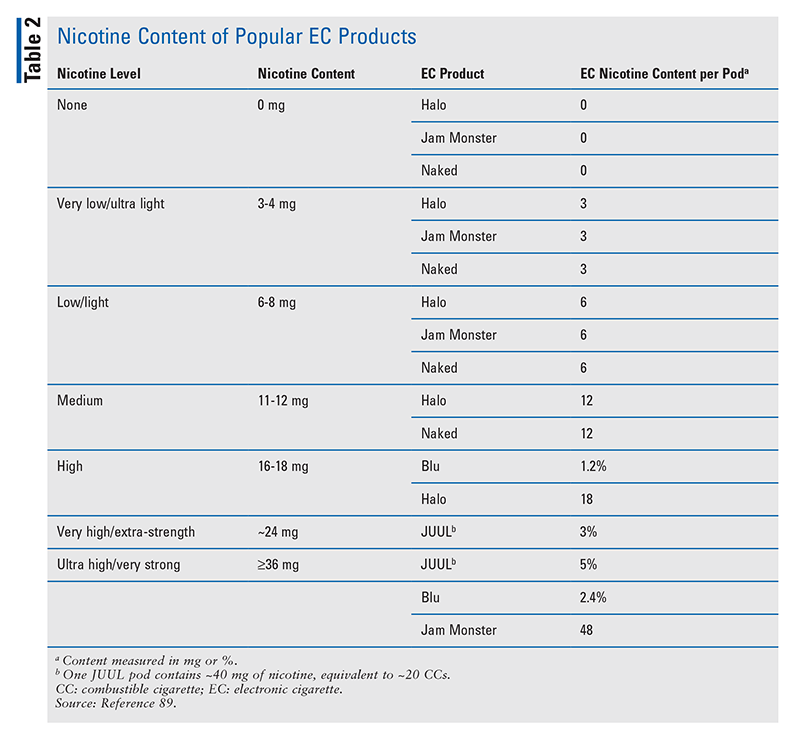
Although patients who use ECs for smoking cessation are more successful at quitting CCs compared with those using NRT, they are more likely to remain on ECs for an extended period of time.85 In motivated adults, the use of ECs in combination with counseling induces CC abstinence more quickly than counseling alone.86 Those who use ECs daily are more successful at quitting CCs than those who use them more infrequently; this is because it helps maintain the behavioral aspects of CC smoking, such as smoking when driving a car or having a cup of coffee.82 Although ECs outperform NRT, they are equally or less effective than current pharmacologic therapies.87 Smoking-cessation programs that incorporate self-help strategies are currently being developed for EC users.88 It is difficult to quantify the amount of nicotine in ECs and make a direct correlation to an equivalent number of CCs. The information in TABLE 2 on the most popular EC brands can help determine appropriate NRT therapy.89 As long-term data regarding the health benefits versus risks of ECs emerge, practice recommendations will likely evolve and become standardized.
REFERENCES
1. Sapru S, Vardhan M, Qianhao L, et al. E-cigarettes use in the United States: reasons for use, perceptions, and effects on health. BMC Public Health. 2020;20:1518.
2. Mayer M, Reyes-Guzman C, Grana R, et al. Demographic characteristics, cigarette smoking, and e-cigarette use among U.S. adults. JAMA Netw Open. 2020;3:e2020694.
3. Pepper JK, Ribisl KM, Emery SL, Brewer NT. Reasons for starting and stopping electronic cigarette use. Int J Environ Res Public Health. 2014;11:10345-10361.
4. Patel D, Davis KC, Cox S, et al. Reasons for current e-cigarette use among U.S. adults. Prev Med. 2016;93:14-20.
5. Dautzenberg B, Bricard D. Real-time characterization of e-cigarettes use: the 1 Million Puffs study. J Addict Res Ther. 2015;6:229.
6. Hussain S, Shahid Z, Foroozesh MB, Sofi UF. E-cigarettes: a novel therapy or a looming catastrophe. Ann Thorac Med. 2021;16:73-80.
7. Goniewicz ML, Miller CR, Sutanto E, Li D. How effective are electronic cigarettes for reducing respiratory and cardiovascular risk in smokers? A systematic review. Harm Reduct J. 2020;17:91.
8. Glantz SA, Bareham DW. E-cigarettes: use, effects on smoking, risks, and policy implications. Annu Rev Public Health. 2018;39:215-235.
9. Darabseh MZ, Selfe J, Morse CI, Degens H. Is vaping better than smoking for cardiorespiratory and muscle function? Multidiscip Respir Med. 2020;15:674.
10. Gentzke AS, Creamer M, Cullen KA, et al. Vital signs: tobacco product use among middle and high school students—United States, 2011-2018. MMWR Morb Mortal Wkly Rep. 2019;68:157-164.
11. FDA. Results from the annual National Youth Tobacco Survey. www.fda.gov/tobacco-products/youth-and-tobacco/youth-tobacco-use-results-national-youth-tobacco-survey. Accessed April 20, 2022.
12. Wang TW, Neff LJ, Park-Lee E, et al. E-cigarette use among middle and high school students—United States, 2020. MMWR Morb Mortal Wkly Rep. 2020;69:1310-1312.
13. Leventhal AM, Strong DR, Kirkpatrick MG, et al. Association of electronic cigarette use with initiation of combustible tobacco product smoking in early adolescence. JAMA. 2015;314:700-707.
14. Soneji S, Barrington-Trimis JL, Wills TA, et al. Association between initial use of e-cigarettes and subsequent cigarette smoking among adolescents and young adults: a systematic review and meta-analysis. JAMA Pediatr. 2017;171:788-797.
15. Berry KM, Fetterman JL, Benjamin EJ, et al. Association of electronic cigarette use with subsequent initiation of tobacco cigarettes in US youths. JAMA Netw Open. 2019;2:e187794.
16. Khouja JN, Suddell SF, Peters SE, et al. Is e-cigarette use in non-smoking young adults associated with later smoking? A systematic review and meta-analysis. Tob Control. 2020;30:8-15.
17. Zhu SH, Gamst A, Lee M, et al. The use and perception of electronic cigarettes and snus among the U.S. population. PLoS One. 2013;8:e79332.
18. Hart EP, Sears CG, Hart JL, Walker KL. Electronic cigarettes and communication: an examination of college students’ perceptions of safety and use. Ky J Commun. 2017;36:35-51.
19. van Staden SR, Groenewald M, Engelbrecht R, et al. Carboxyhaemoglobin levels, health and lifestyle perceptions in smokers converting from tobacco cigarettes to electronic cigarettes. S Afr Med J. 2013;103:865-868.
20. Sears C, Hart J, Walker K, et al. A dollars and “sense” exploration of vape shop spending and e-cigarette use. Tob Prev Cessat. 2016;2(suppl):9.
21. Hoetger C, Bono RS, Nicksic NE, et al. Influence of electronic cigarette characteristics on susceptibility, perceptions, and abuse liability indices among combustible tobacco cigarette smokers and non-smokers. Int J Environ Res Public Health. 2019;16:1825.
22. Herman M, Tarran R. E-cigarettes, nicotine, the lung and the brain: multi-level cascading pathophysiology. J Physiol. 2020;598:5063-5071.
23. Faulcon LM, Rudy S, Limpert J, et al. Adverse experience reports of seizures in youth and young adult electronic nicotine delivery systems users. J Adolesc Health. 2020;66:15-17.
24. Shao XM, Fang ZT. Severe acute toxicity of inhaled nicotine and e-cigarettes: seizures and cardiac arrhythmia. Chest. 2020;157:506-508.
25. Benowitz NL. Seizures after vaping nicotine in youth: a canary or a red herring? J Adolesc Health. 2020;66:1-2.
26. FDA. Some e-cigarette users are having seizures, most reports involving youth and young adults. www.fda.gov/tobacco-products/ctp-newsroom/some-e-cigarette-users-are-having-seizures-most-reports-involving-youth-and-young-adults. Accessed April 20, 2022.
27. Heldt NA, Reichenbach N, McGary HM, Persidsky Y. Effects of electronic nicotine delivery systems and cigarettes on systemic circulation and blood-brain barrier: implications for cognitive decline. Am J Pathology. 2021;191:243-255.
28. Laviolette SR. Molecular and neuronal mechanisms underlying the effects of adolescent nicotine exposure on anxiety and mood disorders. Neuropharmacology. 2021;184:108411.
29. Pepper JK, Brewer NT. Electronic nicotine delivery system (electronic cigarette) awareness, use, reactions and beliefs: a systematic review. Tob Control. 2014;23:375-384.
30. U.S. Department of Health and Human Services (HHS). How Tobacco Smoke Causes Disease: The Biology and Behavioral Basis for Smoking-Attributable Disease. A Report of the Surgeon General. Atlanta, GA: HHS, CDC, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health; 2010.
31. Glasser AM, Collins L, Pearson JL, et al. Overview of electronic nicotine delivery systems: a systematic review. Am J Prev Med. 2017;52:e33-e66.
32. Hajek P, Etter JF, Benowitz N, et al. Electronic cigarettes: review of use, content, safety, effects on smokers and potential for harm and benefit. Addiction. 2014;109:1801-1810.
33. Breitbarth AK, Morgan J, Jones AL. E-cigarettes—an unintended illicit drug delivery system. Drug Alcohol Depend. 2018;192:98-111.
34. Tsai M, Byun MK, Shin J, Crotty Alexander LE. Effects of e-cigarettes and vaping devices on cardiac and pulmonary physiology. J Physiol. 2020;598:5039-5062.
35. Benowitz NL, Fraiman JB. Cardiovascular effects of electronic cigarettes. Nat Rev Cardiol. 2017;14:447-456.
36. Kaur G, Pinkston R, McLemore B, et al. Immunological and toxicological risk assessment of e-cigarettes. Eur Respir Rev. 2018;27:170119.
37. Li Y, Burns AE, Tran LN, et al. Impact of e-liquid composition, coil temperature, and puff topography on the aerosol chemistry of electronic cigarettes. Chem Res Toxicol. 2021;34:1640-1654.
38. National Academies of Sciences, Engineering, and Medicine; Health and Medicine Division; Board on Population Health and Public Health Practice; et al. Public Health Consequences of E-Cigarettes. Washington, DC: National Academies Press; 2018.
39. Kadry H, Noorani B, Bickel U, et al. Comparative assessment of in vitro BBB tight junction integrity following exposure to cigarette smoke and e-cigarette vapor: a quantitative evaluation of the protective effects of metformin using small-molecular-weight paracellular markers. Fluids Barriers CNS. 2021;18:28.
40. Kaisar MA, Sivandzade F, Bhalerao A, Cucullo L. Conventional and electronic cigarettes dysregulate the expression of iron transporters and detoxifying enzymes at the brain vascular endothelium: in vivo evidence of a gender-specific cellular response to chronic cigarette smoke exposure. Neurosci Lett. 2018;682:1-9.
41. Sifat AE, Vaidya B, Kaisar MA, et al. Nicotine and electronic cigarette (E-Cig) exposure decreases brain glucose utilization in ischemic stroke. J Neurochem. 2018;147:204-221.
42. Shah KK, Boreddy PR, Abbruscato TJ. Nicotine pre-exposure reduces stroke-induced glucose transporter-1 activity at the blood-brain barrier in mice. Fluids Barriers CNS. 2015;12:10.
43. Prasad S, Sajja RK, Kaisar MA, et al. Role of Nrf2 and protective effects of Metformin against tobacco smoke-induced cerebrovascular toxicity. Redox Biol. 2017;12:58-69.
44. Sivandzade F, Prasad S, Bhalerao A, Cucullo L. NRF2 and NF-KB interplay in cerebrovascular and neurodegenerative disorders: molecular mechanisms and possible therapeutic approaches. Redox Biol. 2019;21:101059.
45. Ashabi G, Khalaj L, Khodagholi F, et al. Pre-treatment with metformin activates Nrf2 antioxidant pathways and inhibits inflammatory responses through induction of AMPK after transient global cerebral ischemia. Metab Brain Dis. 2015;30:747-754.
46. Kaisar MA, Villalba H, Prasad S, et al. Offsetting the impact of smoking and e-cigarette vaping on the cerebrovascular system and stroke injury: is Metformin a viable countermeasure? Redox Biol. 2017;13:353-362.
47. Son Y, Mishin V, Laskin JD, et al. Hydroxyl radicals in e-cigarette vapor and e-vapor oxidative potentials under different vaping patterns. Chem Res Toxicol. 2019;32:1087-1095.
48. Naik P, Cucullo L. Pathobiology of tobacco smoking and neurovascular disorders: untied strings and alternative products. Fluids Barriers CNS. 2015;12:25.
49. Hawkins BT, Abbruscato TJ, Egleton RD, et al. Nicotine increases in vivo blood-brain barrier permeability and alters cerebral microvascular tight junction protein distribution. Brain Res. 2004;1027:48-58.
50. Hutamekalin P, Farkas AE, Orbók A, et al. Effect of nicotine and polyaromatic hydrocarbons on cerebral endothelial cells. Cell Biol Int. 2008;32:198-209.
51. Das S, Gautam N, Dey SK, et al. Oxidative stress in the brain of nicotine-induced toxicity: protective role of Andrographis paniculata Nees and vitamin E. Appl Physiol Nutr Metabol. 2009;34:124-135.
52. Pryor WA, Stone K. Oxidants in cigarette smoke. Radicals, hydrogen peroxide, peroxynitrate, and peroxynitrite. Ann N Y Acad Sci. 1993;686:12-27.
53. Naik P, Fofaria N, Prasad S, et al. Oxidative and pro-inflammatory impact of regular and denicotinized cigarettes on blood brain barrier endothelial cells: is smoking reduced or nicotine-free products really safe? BMC Neurosci. 2014;15:51.
54. Abbruscato TJ, Lopez SP, Roder K, Paulson JR. Regulation of blood-brain barrier Na,K,2Cl-cotransporter through phosphorylation during in vitro stroke conditions and nicotine exposure. J Pharmacol Exp Ther. 2004;310:459-468.
55. Abbruscato TJ, Lopez SP, Mark KS, et al. Nicotine and cotinine modulate cerebral microvascular permeability and protein expression of ZO-1 through nicotinic acetylcholine receptors expressed on brain endothelial cells. J Pharm Sci. 2002;91:2525-2538.
56. Prasad S, Sajja RK, Park JH, et al. Impact of cigarette smoke extract and hyperglycemic conditions on blood-brain barrier endothelial cells. Fluids Barriers CNS. 2015;12:18.
57. Sivandzade F, Cucullo L. Assessing the protective effect of rosiglitazone against electronic cigarette/tobacco smoke-induced blood-brain barrier impairment. BMC Neurosci. 2019;20:15.
58. Kuntic M, Oelze M, Steven S, et al. Short-term e-cigarette vapour exposure causes vascular oxidative stress and dysfunction: evidence for a close connection to brain damage and a key role of the phagocytic NADPH oxidase (NOX-2). Eur Heart J. 2020;41:2472-2483.
59. Singh KP, Lawyer G, Muthomalage T, et al. Systemic biomarkers in electronic cigarette users: implications for noninvasive assessment of vaping-associated pulmonary injuries. ERJ Open Res. 2019;5:00182-2019.
60. Song K, Li Y, Zhang H, et al. Oxidative stress-mediated blood-brain barrier (BBB) disruption in neurological diseases. Oxidative Med Cellular Longevity. 2020;2020:4356386.
61. Sivandzade F, Alqahtani F, Cucullo L. Traumatic brain injury and blood-brain barrier (BBB): underlying pathophysiological mechanisms and the influence of cigarette smoking as a premorbid condition. Int J Mol Sci. 2020;21:2721.
62. Wharton JD, Kozek LK, Carson RP. Increased seizure frequency temporally related to vaping: where there’s vapor, there’s seizures? Pediatr Neurol. 2020;104:66-67.
63. Klein AP, Yarbrough K, Cole JW. Stroke, smoking and vaping: the no-good, the bad and the ugly. Ann Public Health Res. 2021;8:1104.
64. Vlachopoulos C, Ioakeimidis N, Abdelrasoul M, et al. Electronic cigarette smoking increases aortic stiffness and blood pressure in young smokers. J Am Coll Cardiol. 2016;67:2802-2803.
65. Franzen KF, Willig J, Talavera SC, et al. E-cigarettes and cigarettes worsen peripheral and central hemodynamics as well as arterial stiffness: a randomized, double-blinded pilot study. Vasc Med. 2018;23:419-425.
66. Chaumont M, de Becker B, Zaher W, et al. Differential effects of e-cigarette on microvascular endothelial function, arterial stiffness and oxidative stress: a randomized crossover trial. Sci Rep. 2018;8:10378.
67. Caporale A, Langham MC, Guo W, et al. Acute effects of electronic cigarette aerosol inhalation on vascular function detected at quantitative MRI. Radiology. 2019;293:97-106.
68. Fetterman JL, Keith RJ, Palmisano JN, et al. Alterations in vascular function associated with the use of combustible and electronic cigarettes. J Am Heart Assoc. 2020;9:e014570.
69. Maessen GC, Wijnhoven AM, Neijzen RL, et al. Nicotine intoxication by e-cigarette liquids: a study of case reports and pathophysiology. Clin Toxicol (Phila). 2020;58:1-8.
70. Schaller K, Ruppert L, Kahnert S, et al. Electronic Cigarettes—an Overview. Heidelberg, Germany: German Cancer Research Center; 2013.
71. Zar T, Graeber C, Perazella MA. Recognition, treatment, and prevention of propylene glycol toxicity. Semin Dial. 2007;20:217-219.
72. Jones RD, Asare M, Lanning B. A retrospective cross-sectional study on the prevalence of e-cigarette use among college students. J Community Health. 2021;46:195-202.
73. Leventhal AM, Strong DR, Sussman S, et al. Psychiatric comorbidity in adolescent electronic and conventional cigarette use. J Psychiatr Res. 2016;73:71-78.
74. Tidey JW, Miller ME. Smoking cessation and reduction in people with chronic mental illness. BMJ. 2015;351:h4065.
75. Benowitz NL. Pharmacology of nicotine: addiction, smoking-induced disease, and therapeutics. Annu Rev Pharmacol Toxicol. 2009;49:57-71.
76. Dahal R, Adhikari K, Patten SB. Smoking cessation and improvement in mental health outcomes: do people who quit smoking by switching to electronic cigarettes experience improvement in mental health? Can J Psychiatry. 2020;65:512-514.
77. Lee S, Oh Y, Kim H, et al. Implications of electronic cigarette use for depressive mood: a nationwide cross-sectional study. Medicine (Baltimore). 2020;99:e22514.
78. Obisesan OH, Mirbolouk M, Osei AD, et al. Association between e-cigarette use and depression in the Behavioral Risk Factor Surveillance System, 2016-2017. JAMA Netw Open. 2019;2:e1916800.
79. Simmons VN, Quinn GP, Harrell PT, et al. E-cigarette use in adults: a qualitative study of users’ perceptions and future use intentions. Addict Res Theory. 2016;24:313-321.
80. Orellana-Barrios MA, Payne D, Mulkey Z, Nugent K. Electronic cigarettes—a narrative review for clinicians. Am J Med. 2015;128:674-681.
81. Harrell PT, Marquinez NS, Correa JB, et al. Expectancies for cigarettes, E-cigarettes, and nicotine replacement therapies among e-cigarette users (aka vapers). Nicotine Tob Res. 2015;17:193-200.
82. Wang RJ, Bhadriraju S, Glantz SA. E-cigarette use and adult cigarette smoking cessation: a meta-analysis. Am J Public Health. 2021;111:230-246.
83. Kollath-Cattano C, Dorman T, Albano AW Jr, et al. E-cigarettes and the clinical encounter: physician perspectives on e-cigarette safety, effectiveness, and patient educational needs. J Eval Clin Pract. 2019;25:761-768.
84. Steinberg MB, Zimmermann NH, Delnevo CD, et al. E-cigarette versus nicotine inhaler: comparing the perceptions and experiences of inhaled nicotine devices. J Gen Intern Med. 2014;29:1444-1450.
85. Hajek P, Phillips-Waller A, Przulj D, et al. A randomized trial of e-cigarettes versus nicotine-replacement therapy. N Engl J Med. 2019;380:629-637.
86. Eisenberg MJ, Hébert-Losier A, Windle SB, et al. Effect of e-cigarettes plus counseling vs counseling alone on smoking cessation: a randomized clinical trial. JAMA. 2020;324:1844-1854.
87. Borrelli B, O’Connor GT. E-cigarettes to assist with smoking cessation. N Engl J Med. 2019;380:678-679.
88. Meltzer LR, Simmons VN, Piñeiro B, et al. Development of a self-help smoking cessation intervention for dual users of tobacco cigarettes and e-cigarettes. Int J Environ Res Public Health. 2021;18:23-28.
89. TRC Healthcare. Vaping cessation guide. https://pharmacist.therapeuticresearch.com/Content/Segments/PRL/2019/Dec/Vaping-Cessation-Guide-S1912002. Accessed April 21, 2022.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
To comment on this article, contact rdavidson@uspharmacist.com.






