US Pharm. 2019:44(12):32-35.
Gastrointestinal (GI) discomfort and distress can impact an older adult’s quality of life, but it is frequently unclear, and potentially confusing, as to which changes in GI function are the manifestation of normal aging processes and which are attributed to pathological findings of active disease processes (TABLE 1).1 In addition, when there are multiple comorbidities, there is a less consistent relationship between disease and clinical manifestations in the elderly.2
Further complicating the scenario is the question of whether the presenting GI symptoms are resulting from current medication therapy—either prescription medications or the OTC drugs frequently encountered in geriatric practice—and are therefore classified as medication-related problems (MRPs). Often mistaken for symptoms of an organic disease, MRPs frequently lead to multiple diagnostic studies.3 Consequences of GI-related drug toxicity are variable and can range across a spectrum from the mild discomfort of drug-induced diarrhea to fatal GI hemorrhage or per-foration; associated morbidity, mortality, and medical costs are probably underestimated.3
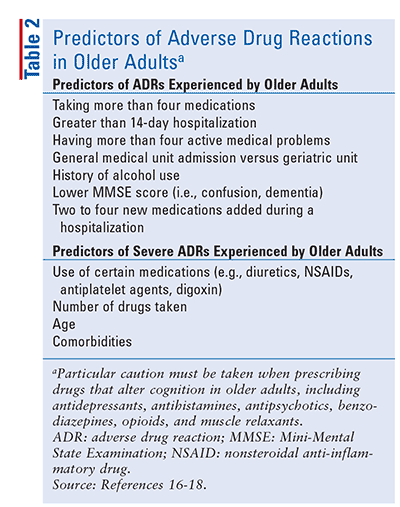
Since older adults in the United States use a disproportionate number of medications, and the number of medications has been shown to be a strong predictor for MRPs (TABLE 2), older adults are clearly at greater risk.4 With the growth of the older-adult population projected to accelerate in the coming decades, it is important for pharmacists to gain a better understanding of the most frequent diseases and MRPs occurring in individuals living to advanced old age. Addressing the safety, appropriateness, and effectiveness of medications in a comprehensive fashion through medication therapy management, pharmacists can provide insight and a nuanced approach to identifying, resolving, and preventing conditions associated with medication-related causative factors.
Although there is no known specific GI disease of the older-adult population, the aging process does result in clinically significant effects on oropharyngeal motility, upper-esophageal motility, colonic function, and GI immunity.2 Additionally, the prevalence of GI symptoms and signs has increased, owing to aging processes and to the additional effects of comorbidities and environmental exposure (e.g., medications, alcohol, tobacco).2 In particular, tobacco has the potential to increase the risk associated with other carcinogenic agents: For example, alcohol consumption, associated with esophageal cancer, carries a greater risk when combined with cigarette smoking.5
Aging is characterized by changes occurring in the structure, motility, coordination, and sensitivity of the swallowing process, and it has been estimated that 35% to 68% of people aged 65 years and older have some degree of swallowing dysfunction.6-8 The swallowing process is divided into three stages: 1) oral stage (voluntary); 2) pharyngeal stage; 3) esophageal stage; this discussion will provide an overview of the characteristics of the oral cavity and oropharyngeal and esophageal disorders in older adults, raising awareness of medication-related contributors.
Oral Cavity and Swallowing Dysfunction
The most commonly reported disturbances of the oral cavity among older individuals include oral sensorial complaints (OSCs), particularly dry mouth (xerostomia), taste disturbances (dysgeusia or ageusia), and burning-mouth syndrome (TABLE 1).9 OSCs are more prevalent in adults aged 65 years and older; 50% of older-adult patients report at least one OSC, with those using prescription drugs having a higher prevalence of OSCs.9,10
With regard to swallowing, this physiologic process requires a complex series of psychological, sensory, and motor functions that are both voluntary and involuntary.11 TABLE 3 outlines age-related causes of swallowing dysfunction in older adults of which pharmacists should be aware in order to determine appropriateness of therapy and better guide patients regarding medication administration along the age continuum.
Esophagus
Esophageal problems in the older adult are more closely aligned with other comorbidities rather than with the esophagus itself.1 Medication-induced esophagitis is inflammation of the esophagus secondary to harmful effects of medication produced by 1) altered passage through the esophagus and 2) increased contact with esophageal mucosa.1 This esophageal injury may be referred to as pill esophagitis (PE), because pills commonly lodge in the esophagus (i.e., at the level of the aortic knob or the lower esophageal sphincter), unknown to the patient. This medication-related adverse effect is more prevalent in older adult patients than in any other patient age group.12 The most common symptoms of PE are retrosternal (chest) pain (71.8%) and odynophagia (38.5%).13 The most common contributing factors of medication-induced esophagitis in the elderly include 1) polypharmacy; 2) decrease in esophageal motility; and 3) taking medication with insufficient amounts of water.14 Furthermore, patients with cardiomegaly can develop esophageal compression from an enlarged left atrium, placing them at increased risk for medication-induced esophagitis. In addition to advanced age, Abid and colleagues found female gender, presence of diabetes, and ischemic heart disease to be associated with medication-induced esophagitis.14
Role of the Pharmacist
Although a number of pharmacologic agents are associated with medication-induced esophagitis, selected commonly involved causative agents are listed in TABLE 4. Detailed history, availability of accurate medication list, and endoscopy are invaluable in establishing the diagnosis of esophagitis.1 Endoscopic findings show ulceration in more than 80% of cases, while kissing ulcers (ulcers facing each other) are present in up to 42% of patients.13 Pharmacists should not underestimate the importance of taking the time to instruct older adult patients and caregivers about the seriousness of taking a solid oral dosage form (i.e., pills) with a generous amount of water (e.g., 180 mL) and to avoid lying down for at least 30 minutes after administration; there is a decrease in esophageal motor activity and a decrease in salivation during sleeping.15 The mainstay of treatment of medication-induced esophagitis is withdrawal of the inciting medication and use of proton-pump inhibitors, leading to a favorable prognosis in most cases.1
Conclusion
The prevalence of GI symptoms and signs has increased, owing to aging processes and to the effects of comorbidities and environmental exposure (medications, alcohol, tobacco). Since age-related physiologic changes in the GI tract, as in most systems, affect diagnostic test interpretation and response to treatments—and as the number of older adults will continue to increase in the coming decades—age-related changes in GI function and GI morbidity in the elderly represent an increasingly important burden for public health.2 Better awareness of the potential for medication-induced GI-tract disease by healthcare practitioners improves the recognition of these adverse drug reactions. (ADRs), and ultimately, improves patient care.3 Pharmacists should do all they can to provide appropriately effective recommendations, monitoring, and patient counseling and guidance to address preventable medication-related causes, focusing on issues with polypharmacy, one of the predictors of ADRs.
REFERENCES
1. Dumic I, Nordin T, Jecmenica M, et al. Gastrointestinal tract disorders in older age. Can J Gastroenterol Hepatol. 2019;2019:6757524.
2. Durazzo M, Campion D, Fagoonee S, Pellicano R.. Gastrointestinal tract disorders in the elderly. Minerva Med. 2017;108(6):575-591.
3. Jain V, Pitchumoni CS. Gastrointestinal side effects of prescription medications in the older adult. J Clin Gastroenterol. 2009;43(2):103-110.
4. Steinman MA, Miao Y, Boscardin WJ, et al. Prescribing quality in older veterans: a multifocal approach. J Gen Intern Med. 2014;29(10):1379-1386.
5. Yang X, Chen X, Zhuang M, et al. Smoking and alcohol drinking in relation to the risk of esophageal squamous cell carcinoma: a population-based case-control study in China. Sci Rep. 2017;7:17249.
6. Nilsson H, Ekberg O, Olsson R, Hindfelt B. Quantitative aspects of swallowing in an elderly nondysphagic population. Dysphagia. 1996;11:180-184.
7. Lindgren S, Janzon L. Prevalence of swallowing complaints and clinical findings among 50-79-year-old men and women in an urban population. Dysphagia. 1991;6:187-192.
8. Carnaby-Mann G, Crary M. Pill swallowing by adults with dysphagia. Arch Otolaryngol Head Neck Surg. 2005;131:970-975.
9. Nagler RM, Hershkovich O. Relationships between age, drugs, oral sensorial complaints and salivary profile. Arch Oral Biol. 2005;50(1):7-16.
10. Nagler RM, Hershkovich O. Age-related changes in unstimulated salivary function and composition and its relations to medications and oral sensorial complaints. Aging Clin Exp Res. 2005;17(5):358-366.
11. Fusco S, Cariati D, Schepisi R, et al. Management of oral drug therapy in elderly patients with dysphagia. J Genetics Genomics. 2016;64:9-20.
12. Kikendall JW. Pill-induced esophagitis. Gastroenterol Hepatol (NY). 2007;3(4):275-276.
13. Kim SH, Jeong JB, Kim JW, et al. Clinical and endoscopic characteristics of drug-induced esophagitis. World J Gastroenterol. 2014;20(31):10994-10999.
14. Abid S, Mumtaz K, Jafri W, et al. Pill-induced esophageal injury: endoscopic features and clinical outcomes. Endoscopy. 2005;37(8):740-744.
15. Zografos GN, Georgiadou D, Thomas D, et al. Drug-induced esophagitis. Dis Esophagus. 2009;22:633-637.
16. Lee JK, Mendoza DM, Mohler MJ, et al. Geriatrics. In: Chisholm-Burns MA, Schwinghammer TL, Malone PM, et al, eds. Pharmacotherapy: Principles & Practice, 5th ed. New York, NY: McGraw Hill Education; 2019:7-18.
17. Gurwitz JH, Field TS, Harrold LR, et al. Incidence and preventability of adverse drug events among older persons in the ambulatory setting. JAMA. 2003;289:1107-1116.
18. Merle L, Laroche ML, Dantoine T, Charmes JP. Predicting and preventing adverse drug reactions in the very old. Drugs Aging. 2005;22(5):375-392.
19. Robbins J, Levine R, Wood J, et al. Age effects on lingual pressure generation as a risk factor for dysphagia. J Gerontol A Biol Sci Med Sci. 1995;50:M257-M262.
20. Nagaya M, Sumi Y. Reaction time in the submental muscles of normal older people. J Am Geriatr Soc. 2002;50:975-976.
21. Clave P, Arreola V, Romea M, et al. Accuracy of the volume-viscosity swallow test for clinical screening of oropharyngeal dysphagia and aspiration. Clin Nutr. 2008;27:806-815.
22. Jou J, Radowsky J, Gangnon R, et al. Esophageal clearance patterns in normal older adults as documented with videofluoroscopic esophagram. Gastroenterol Res Pract. 2009;2009:965062.
23. Hind JA, Nicosia MA, Roecker EB, et al. Comparison of effortful and noneffortful swallows in healthy middle-aged and older adults. Arch Phys Med Rehabil 2001;82:1661-1665.
24. Ney DM, Weiss JM, Kind AJ, Robbins J. Senescent swallowing: impact, strategies, and interventions. Nutr Clin Pract. 2009;24:395-413.
25. Shiozu H, Higashijima M, Koga T. Association of sarcopenia with swallowing problems, related to nutrition and activities of daily living of elderly individuals. J Phys Ther Sci. 2015;27:393-396.
26. Stokely SL, Peledeau-Pigeon M, Leigh C, Xee L. The relationship between pharyngeal constriction and post-swallow residue. Dysphagia.2015;30(3):349-356.
27. Zhang Yu, Tong Y, Wang W, et al. Chest pain from pill-induced esophagitis: a rare side effect of ascorbic acid. SAGE Open Med Case Rep. 2018;6:2050313X18775004.
28. de Groen PC, Lubbe DF, Hirsch LJ, et al. Esophagitis associated with the use of alendronate. N Engl J Med. 1996;335:1016-1021.
To comment on this article, contact rdavidson@uspharmacist.com.








