US Pharm. 2020;45(1):30-33.
ABSTRACT: Occipital neuralgia is a rare type of headache that can present like migraine, with unilateral, throbbing pain, especially when it radiates to the frontal, orbital, and periorbital region. Irritation of the greater and/or lesser occipital nerves by chronically contracted muscles and spondylosis of the upper cervical spine is often implicated. Treatment options include first-line, conservative management with physical therapy and noninvasive pharmacotherapy; second-line treatments include steroid injections, botulinum toxin infiltrations, and pulsed radiofrequency; surgical options include neurolysis of the occipital nerve and occipital nerve stimulation.
Occipital neuralgia (ON) is a challenging diagnosis. ON, also known as Arnold’s neuralgia, is defined by the International Headache Society as a unilateral or bilateral paroxysmal, shooting, or stabbing pain in the posterior part of the scalp, in the distribution of the greater occipital nerve (GON), lesser occipital nerve (LON), or third occipital nerve, sometimes accompanied by diminished sensation or dysesthesia in the affected area and commonly associated with tenderness over the involved nerve(s).1 Pain classically originates in the suboccipital region and radiates toward the posterior and/or lateral scalp over the vertex; however, pain may also be perceived retro-orbitally and over the neck, temple, and frontal regions. Pain intensity is often severe and debilitating, with an associated negative impact upon quality of life and function. The GON is more frequently involved (90%), whereas the LON is less frequently involved (10%). Both the GON and LON are involved in 8.7% of cases (10%).2
The incidence of ON remains to be accurately determined. In one study investigating the incidences of facial pain in a Dutch population, ON comprised 8.3% of facial-pain cases. The total incidence of ON was 3.2 per 100,000 people, with a mean age at diagnosis of 54.1 years.3
ETIOLOGY
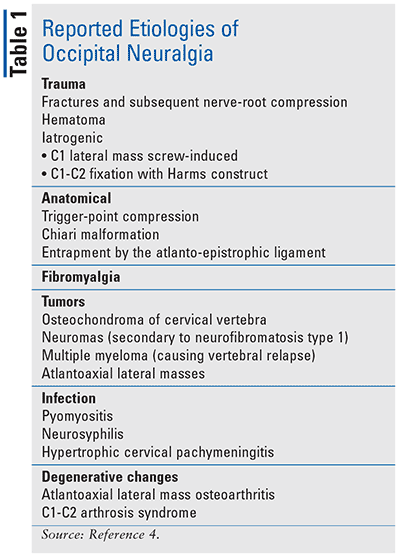
Neuralgia is pain in one or more nerves caused by compression and/or irritation of peripheral-nerve structures. In ON, irritation of the GON and/or LON by chronically contracted muscles and spondylosis of the upper cervical spine is often implicated. ON is considered to be idiopathic in nature; however, several etiologies have been described in the development of ON, including trauma (e.g., motor vehicle accident “whiplash”), compression (e.g., atlantoaxial instability secondary to degenerative changes), or nerve entrapment (myofascial or vascular). TABLE 1 summarizes the various etiologies implicated in ON. Some rare cases of ON include schwannomas and other neoplastic processes, postherpetic neuralgia, and temporal arteritis.4,5
DIAGNOSIS
After completing a focused history and physical examination, the diagnosis is confirmed by local anesthetic blockade of the suspected nerve. The patient should have pain relief with the nerve block for at least the duration of the local anesthetic. Single diagnostic blocks carry false-positive rates up to 40%, so it is prudent to perform a second block. Because compression is thought to be the main etiology for ON, imaging should be considered if there is suspicion of lesion or mass at the affected area.3
ON can present like migraine, with unilateral, throbbing pain, especially when it radiates to the frontal, orbital, and periorbital region. Sometimes nausea, vomiting, photophobia or phonophobia, and eye changes may accompany ON and mimic a migraine. The situation is further complicated by the ability of occipital nerve blocks to relieve migraine headaches and the fact that both these disorders seem to coexist. One way to distinguish between the two is that typical acute treatments for migraine, such as triptans or ergot alkaloids, will not work for ON.3,6
TREATMENT OPTIONS
Conservative Management: First-Line Treatment
First-line treatment consists of conservative management, including rest, massage, hot/cold compresses, and physical therapy. An escalation of care can include anti-inflammatory medications and muscle relaxants, especially in the context of acute pain. Nonsteroidal anti-inflammatory drugs and acetaminophen tend to have transient effects. In instances in which the pain is chronic, a trial of antiepileptics, antidepressants, or GABA-targeted therapies may be initiated. ON is difficult to treat because symptoms often don’t respond to these traditional treatments.5-7
Interventional Management: Second-Line Treatment
For those patients whose ON pain is resistant to conservative therapies, more invasive measures may be considered, including steroid injections (dexamethasone), local anesthetic nerve blocks (lidocaine and bupivacaine), and botulinum A toxin injection. Although these procedures do have relatively high initial success rates, limitations include the need for repeat injections and loss of efficacy over time.5
Local Anesthetic Agent Injection: This may be done with or without a steroid. The rationale for injecting local anesthetics (LA) is to block sensory signals from the region being injected. Although often used for diagnosis—because it should only lead to a temporary blockade—an injection of LA has the potential to decrease sensitization, which is a feature of chronic or persistent pain, thereby possibly prolonging the treatment effect of LA beyond its pharmacologic duration of action.8
Botulinum Toxin Infiltrations: Although there is not yet enough evidence to demonstrate efficacy of botulinum neurotoxin toxin A (BoNT/A) for ON, two small studies have shown some positive results. A retrospective case series involving six patients with ON who received occipital nerve blocks with 50 units of BoNT/A found pain- and disability-index improvement in five out of six patients. Pain relief persisting for more than 4 months was reported in five patients. A retrospective pilot study of six patients with ON treated with BoNT/A with 12-week follow-up showed improvement in sharp, shooting pain and pins-and-needles headache pain but no significant improvement in dull, aching pain and no reduction in pain-medication use.9
Pulsed Radiofrequency: Depending on how radiofrequency energy is applied to neural tissues, radiofrequency therapy can be defined as thermal or pulsed. Investigators have studied the use of pulsed radiofrequency (PRF), a nondestructive form of radiofrequency therapy for the treatment of ON. Several studies of occipital nerve PRF have shown statistically significant improvements in pain scores and quality of life and reductions in pain-medication use. One study compared the effects of PRF to occipital nerve blocks with steroids in a randomized, double-blind study and found PRF to be superior in terms of average pain score reductions at 6 weeks through 6 months.10,11
Given these findings, the researchers suggest that PRF should be considered as a treatment modality for prolonged benefit beyond occipital-nerve blocks using steroids. Thermal rediofrequency therapy produces more heat that results in neural disruption via the creation of a destructive lesion. PRF, in comparison, delivers short bursts of high-amplitude current between comparatively long pauses that allow for the dissipation of heat. Neural tissue is preserved by allowing this heat to dissipate, as demonstrated in histologic studies. Bleeding and infection are rare complications. Hematoma may occur just under the skin or in the deeper muscle layers. Vasovagal reaction may occur during the procedure. Mechanical nerve-root damage can occur from needle trauma but is rare.10,11
Surgery: Last Resort
Surgical treatment of ON can be considered when a patient does not respond adequately to medical therapies, such as repeated injections, or minimally invasive procedures, such as PRF treatment.10
Neurolysis of the Occipital Nerve: Entrapment of the GON in its peripheral course is a significant pathology in ON. Neurolysis of the GON appears to provide safe, durable pain relief in selected patients having chronic headaches caused by ON. Chemical neurolysis with alcohol or phenol carries the same risks as thermal radiofrequency; hypesthesia, dysesthesia, anesthesia dolorosa, and painful neuroma formation. Neurolysis of the ON is irreversible. In one retrospective pilot study of 206 patients who had ON treated with neurolysis with 12-month follow-up, neurolysis was shown to provide greater than 50% pain relief, a decrease in the consumption of all analgesics, and improvement in overall patient satisfaction.3,7
Occipital Nerve Stimulation: Occipital nerve stimulation (ONS) is a form of neuromodulation therapy aimed at treating intractable headache and craniofacial pain. This stimulation technique involves the SC insertion of electrodes in the C1-C2 region of the posterior cervical spine. The presumed mechanisms of action involve modulation of the trigeminocervical complex, as well as closure of the physiologic pain gate. As opposed to destructive surgery, ONS is fully reversible. If the patient does not want to use stimulation, it is easy to stop the stimulation, and the device can be removed with a simple procedure. Complications may occur, including lead migration, infection, wound erosion, device failure, muscle spasms, and pain.7,12
Other Destructive Surgeries: As in other conditions, the treatment of ON proceeds from least to most invasive. Although C2 gangliotomy, C2 ganglionectomy, C2 to C3 rhizotomy, C2 to C3 root decompression, and distal neurectomy have, been tried, historically, for intractable cases, these kinds of destructive surgeries risk the development of painful neuroma, causalgia, or intractable neuropathic pain, and thus their use is decreasing.7
CONCLUSION
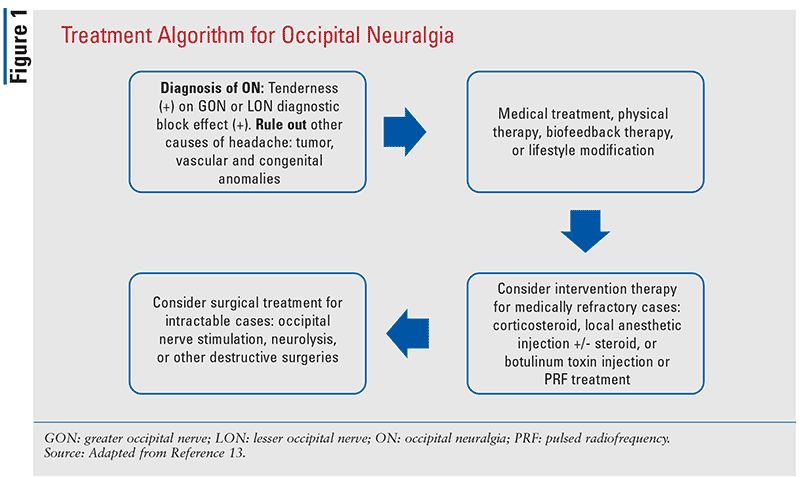
ON is a headache syndrome that requires careful attention to enable proper diagnosis and treatment. Typically, there is no clear structural cause, although appropriate workup should be considered in order to rule out pathologic structural causes. The treatment of ON should be performed using an adequate algorithm (FIGURE 1). Pharmacotherapy is based on the use of antidepressants and antiepileptic drugs, along with topical treatments. If the pain persists despite preliminary therapies and occipital nerve blockade with local anesthetic and steroid, then botulinum toxin or permanent implantation of a percutaneous occipital nerve stimulator should be considered before destructive C2 and/or C3 root surgical procedures are implemented.6,7,13,14
It is natural to expect that as a patient progresses through various stages of treatment, several providers will be involved, such as primary care physicians and physician-extenders, neurologists, pain management physicians, and neurosurgeons. Pharmacists are uniquely positioned to provide counseling, referrals, and guidance on OTC pain medications and prescription medications used in the management of ON.3,15
REFERENCES
1. International Headache Society. The International Classification of Headache Disorders. 3rd ed. Occipital neuralgia. July 29, 2016. https://ichd-3.org/. Accessed December 26, 2019.
2. Manolitsis N, Elahi F. Pulsed radiofrequency for occipital neuralgia. Pain Physician. 2014;17(6):E709-E717.
3. Djavaherian DM, Guthmiller KB. Occipital neuralgia. StatPearls [Internet]. January 2019. Updated June 4, 2019. www.ncbi.nlm.nih.gov/books/NBK538281/. Accessed December 20, 2019.
4. Cesmebasi A, Muhleman MA, Hulsberg P, et al. Occipital neuralgia: anatomic considerations. Clin Anat. 2015;28(1):101-108.
5. Keifer OP Jr, Diaz A, Campbell M, et al. Occipital nerve stimulation for the treatment of refractory occipital neuralgia: a case series. World Neurosurg. 2017;105:599-604.
6. Sahai-Srivastava S, Macwan S. Atypical facial neuralgias. Pract Pain Manag. 2004;4(6).
7. Choi I, Jeon SR. Neuralgias of the head: occipital neuralgias. J Korean Med Sci. 2016;31(4):479-488.
8. Shanthanna H, Busse JW, Thabane L, et al. Local anesthetic injections with or without steroid for chronic non-cancer pain: a protocol for a systematic review and meta-analysis of randomized controlled trials. Syst Rev. 2016;5:18.
9. Oh HM, Chung ME. Botulinum toxin for neuropathic pain: a review of the literature. Toxins (Basel). 2015;7(8):3127-3154.
10. Hoffman LM, Abd-Elsayed A, Burroughs TJ, Sachdeva H. Treatment of occipital neuralgia by thermal radiofrequency ablation. Ochsner J. 2018;18(3):209-214.
11. Mammis A, Agarwal N, Mogilner AY. Occipital nerve stimulation. Adv Tech Stand Neurosurg. 2015;42:23-32.
12. Barna S, Hashmi M. Occipital neuralgia. Pain Manag Rounds. 2004;1(7):1-6.
13. Dworkin RH, O’Connor AB, Audette J, et al. Recommendations for the pharmacological management of neuropathic pain: an overview and literature update. Mayo Clin Proc. 2010;85(3 Suppl):S3-S14.
14. Rosenthal RM. Use of pulsed radiofrequency in clinical practice. Pract Pain Manag. 2009;9(5):11-18.
15. Santos AP, Mesquita AR, Oliveira KS, Lyra DP Jr. Assessment of community pharmacists’ counselling skills on headache management by using the simulated patient approach: a pilot study. Pharm Pract (Granada). 2013;11(1):3-7.
To comment on this article, contact rdavidson@uspharmacist.com.